PSQH Quick Poll 2025: Taking the Pulse of Infection Prevention Efforts
By Jay Kumar
As part of PSQH’s celebration of International Infection Prevention Week, we decided to reach out to our readers with a few questions to find out the state of infection prevention efforts.
The Quick Poll had a total of 127 respondents. Thanks to our sponsor Inovalon.
Infection prevention efforts
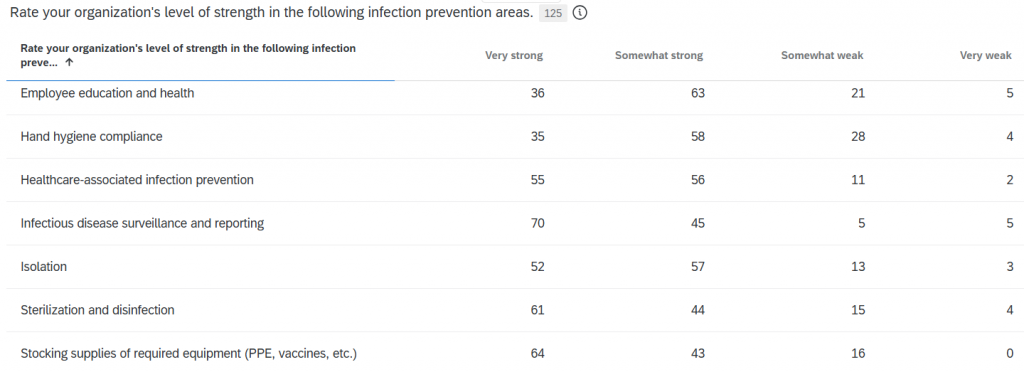
Asked to rate the infection prevention efforts of their organization, 44% of respondents said their program was very effective (down from 51% last year), 52% said their organization’s infection prevention was somewhat effective (up from 49% last year), and 4% said their program was not effective.
Organizational preparedness for infectious disease outbreaks
Flu season is here and COVID-19 remains a concern along with other viruses. From an organizational standpoint, 49% of respondents to the PSQH Quick Poll said they are very prepared for infectious disease outbreaks (down from 58% last year). Another 45% said they are somewhat prepared for future outbreaks (up from 42% last year) and 6% said they are not prepared.

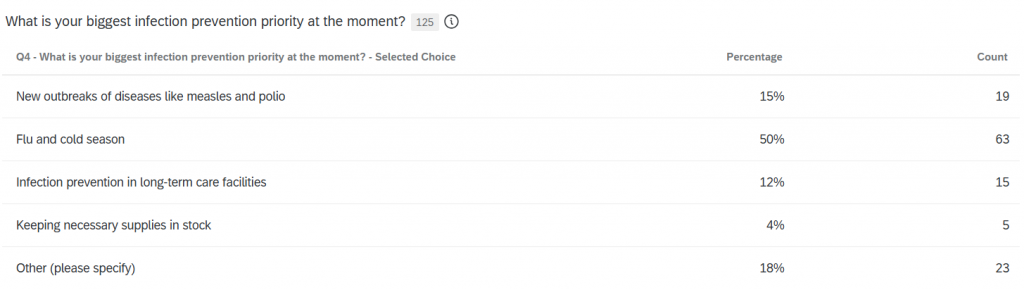
Strength in various infection prevention areas
We queried respondents on their perceived level of strength in various infection control areas. When it comes to healthcare-associated infection prevention, 55% of respondents say they are very strong (43% last year), 56% say they’re somewhat strong (51% last year), and 11% say they are somewhat weak (6.9% last year). With hand hygiene compliance, 35% of respondents say they are very strong (26% in 2024), 58% say they are somewhat strong (51.4% last year), 28% consider themselves somewhat weak (20.6% last year), and 4% say they are very weak (2.5% a year ago).
Infectious disease surveillance and reporting was the strongest area, with 70% of respondents saying they were very strong (56.2% last year), 45% saying they were somewhat strong (37.7% in 2024), and 5% saying they were somewhat weak (6.2% in 2024).
In the area of employee education and health, 36% say they are very strong (33.6% last year), 63% say they are somewhat strong (53.4%), 21% say they are somewhat weak (11.6%), and 5% say they are very weak (1.4%). With regards to isolation, 52% say they are very strong (37.7%), 57% say they are somewhat strong (48.6%), 13% say they are somewhat weak (10.3%), and 3% say they are very weak (1.4%). In sterilization and disinfection, 61% say they are very strong (43.8%), 44% say they are somewhat strong (40%), 15% say they are somewhat weak (8.2%), and 4% say they are very weak (0.7%).
Asked about stocking supplies of required equipment (PPE, vaccines, etc.), 64% say they were very strong (50.7%), 43% say they were somewhat strong (40.4%), and 16% say they were somewhat weak (8.2%).
Biggest priority
Asked about their biggest infection prevention priority at the moment, 50% of respondents say it was flu and cold season. Another 15% say new outbreaks of diseases like measles and polio, 12% say infection prevention in long-term care facilities, and 4% say keeping necessary supplies in stock. Other write-in responses included: to educate and train healthcare workers, consistency with the basic prevention measures, CLABSI prevention, community spread and colonization, HAI prevention, continue to reduce utilization days for foley catheters, handwashing compliance and consistency, Abx stewardship and staff education, HIV PeP policy update, pest control, maintaining regulatory compliance (IFUs), getting buy-in from HCP and staff on the importance of infection prevention, surgical site infections/MDROs, transport of reusable medical devices, building IP program, compliance with hand hygiene, PPE, and disinfection of shared equipment.
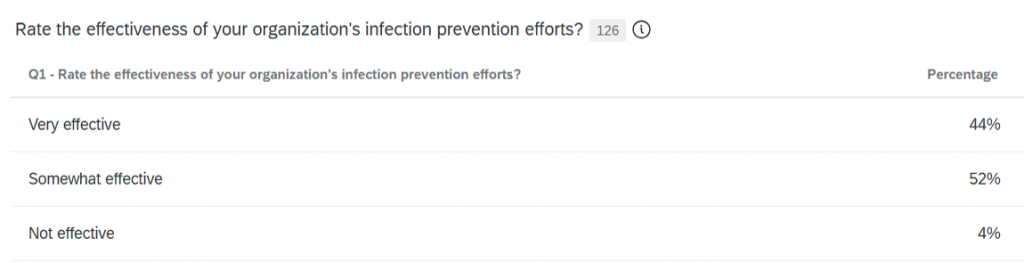
Leadership support for infection prevention
Asked to rate the amount of leadership support for infection prevention, 38% of respondents say it was above and beyond average (vs. 36% in 2024), 48% say it was adequate (56% last year), and 14% say it was lacking (8% a year ago). When respondents were asked how leaders could show more support, 40% say more personnel (45% last year), 34% say increased financial support (27% in 2024), and 6% say more supplies (same as last year). Other write-in responses include: standardized strategy, compliance with policy & procedure, accountability, education to physicians for hand hygiene as they are frequently getting observed for non-compliance, support to address issues related to HAIs/IP, recognize the importance and complexity of infection prevention, more training for the infection prevention coordinator, combination personnel and educational money, engaging with Infection Control, and more training.