Improving Safety and Reducing Harm from Fluoroscopy
By A. Kyle Jones, PhD, DABR; Alexander S. Pasciak, PhD, DABR
Fluoroscopy is a powerful tool that has been used over the past century in many medical disciplines. If asked, ”What is an X-ray?”, many patients would say it is like a photograph—a picture of a body taken at a moment in time. Following this analogy, if a conventional X-ray is similar to a photograph, fluoroscopy is like a video. Instead of capturing only a moment in time, fluoroscopy shows the movement of catheters, devices, and contrast within the body over an extended period of time as part of a procedure performed directly by a physician. Fluoroscopically-guided interventions (FGI) refers to specific uses of fluoroscopy where devices or instruments are inserted through the skin (i.e., percutaneously) and are guided using fluoroscopy to complete a medical procedure.
Simple examples include epidural steroid injections for back pain, often performed with fluoroscopic guidance. Advanced procedures such as percutaneous coronary interventions to treat heart disease and embolization procedures for treatment of cancer or to stop hemorrhage can only be performed using fluoroscopic guidance. These procedures have demonstrated benefits in that they are often outpatient procedures with substantially reduced recovery time and less morbidity than open surgical alternatives. However, safely performing such procedures often requires extensive use of fluoroscopy, which exposes the patient to the risk of skin injury from radiation.
Hundreds of cases of radiation-induced injury resulting from FGI have been reported in the literature over the past 20 years (Koenig, Mettler et al., 2001; Henry et al., 2009; Shope, 1996; Ukisu, Kushihashi, & Soh, 2009; De Olazo Banaag & Carter, 2008). These injuries range in severity from mild redness of the skin to debilitating ulceration and necrosis. The most severe injuries may never heal completely even with multiple surgical interventions. Despite the risks to patients from fluoroscopy, national regulations are notably absent. This is due in large part to the fact that fluoroscopy is unique in diagnostic imaging in that only the dose rate in fluoroscopy is controlled by the equipment configuration, and the total dose is controlled by the physician performing the procedure.
In July of this year, new Joint Commission diagnostic imaging standards will go into effect, which address all advanced medical imaging modalities except fluoroscopy. These standards follow a Sentinel Event Alert issued by The Joint Commission in 2011 that also did not address fluoroscopy. This is unfortunate because injuries from FGI are usually preventable. A simple regulation requiring hospitals and imaging centers to establish a patient safety program in fluoroscopy, focusing primarily on increased awareness of and education of doctors and staff, would markedly reduce the risk.
Background
The first tissue effects from fluoroscopy were observed and reported in 1896. The potential dangers to patients from modern fluoroscopy have been recognized since 1994, when the United States Food and Drug Administration (FDA) Center for Devices and Radiological Health issued a Public Health Advisory alerting physicians and other healthcare professionals to the potential for severe radiation skin burns from fluoroscopically guided procedures. Since then, numerous professional societies and standards organizations have recognized the need for guidelines for their members to improve patient safety during FGI. These include the Society for Interventional Radiology (SIR), the American College of Cardiology (ACC), the National Council on Radiation Protection and Measurements (NCRP), the International Commission on Radiological Protection (ICRP), and the International Atomic Energy Agency (IAEA).
Despite these recommendations, most physicians and administrators are unaware of the potential danger from FGI and have made no effort to implement policies and procedures related to patient safety during FGI. Many of those who are aware of the potential risks to patients from fluoroscopy point to their years of clinical experience as sufficient to ensure safety, however, in Report No. 168 the NCRP states, “Clinical training and experience is not an acceptable substitute for formal training in radiation management” (2011).
 |
|
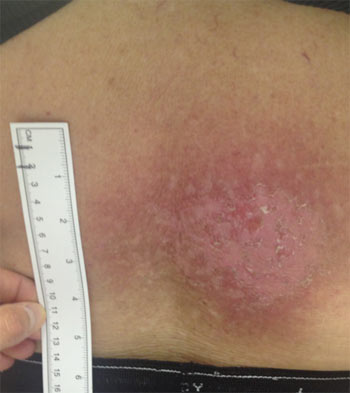
| Figure 1: An example of main erythema 10 weeks after a hepatic embolization procedure. Mild hyperplasia is seen as the skin begins to repopulate. The peak skin dose was estimated to be 10 Gy for this case. |
|
 |
|
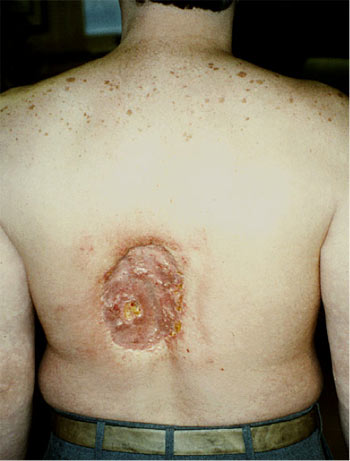
| Figure 2: Deep tissue necrosis 18 to 21 months following FGI. The peak skin dose was estimated to be > 20 Gy in this case. Source: United States Food and Drug Administration. |
Radiation skin injury occupies a spectrum of severity, ranging from mild reddening of the skin (erythema, Figure 1) to ulceration and necrosis in a full-thickness injury (Figure 2), and occasionally injury to the bone—osteoradionecrosis—in the most severe cases (Ukisu, Kushihashi, & Soh, 2009; De Olazo Banaag & Carter, 2008). Very high radiation doses to the skin cause the most severe, debilitating injuries, such as ulceration and necrosis.
The use of such doses of radiation is seldom justified and often results when operators have no formal training on the safe use of fluoroscopy and are unaware of how much radiation they have used and its potential consequences. These types of injuries are most likely to occur when there are no policies and procedures in place that require intra-procedure dose monitoring (NCRP 2014). However, occasionally, the delivery of high radiation doses is justified, particularly for life-saving interventions performed on unstable patients. Radiation skin injury may be an acceptable complication in these cases, however, principles of dose management should still be applied to minimize the severity of the expected injury.
Comparing management of ionizing radiation to the management of iodine contrast is a useful analogy that helps many physicians understand the concept of radiation management. Providers are trained to understand the risks associated with the use of iodine contrast and to understand patient-specific risk factors, such as impaired renal function, that sensitize patients to renal injury from the use of iodine contrast. The volume of iodine contrast used is tracked throughout the procedure, and at the end of the procedure physicians are always cognizant of how much iodine contrast has been used. While the same principles can be applied directly to the management of ionizing radiation, few providers do so. Perhaps the main reason for this disconnect is the knowledge gap that exists for both physicians and administrators regarding the risks associated with and the safe use of fluoroscopy.
Most procedures that result in preventable radiation skin injuries have a number of characteristics in common:
- The patient was not informed that radiation skin injury was a potential risk from the procedure.
- No efforts were made to manage radiation during the procedure.
- The physician was not aware of how much radiation had been used when the case concluded.
- The physician was not aware that skin injury was a potential complication of lengthy FGI.
- The injury was not initially recognized as a radiation skin injury.
While the physical configuration and design of fluoroscopic imaging equipment is heavily regulated in many states, the clinical use of fluoroscopy is not. Administrators may take comfort in meeting regulatory requirements; however, in most cases these requirements do nothing to prevent patient injury. Prevention of injury in fluoroscopy is entirely in the hands of the physician, who may have no formal training on the safe use of fluoroscopy. As a result, hospitals are exposed to tremendous risk if all they do is simply meet existing regulatory requirements.
Compliance with regulations often provides a false sense of security for administrators regarding risk and legal exposure. Patient skin injury has occurred during FGI in states with regulations requiring, among other standards, the recording of radiation dose metrics from fluoroscopy procedures. In the last few years, in our roles as diagnostic medical physicists, we have reviewed cases of extremely high single doses of radiation during FGI, in which the doses were listed in the radiology report but no comment was made as to the magnitude of the doses or the plan for patient management. We have also reviewed a case of an elective procedure that was discovered to be more complicated than expected and resulted in patient harm. The first session was stopped after (presumably) the radiologist became tired, and the case was resumed less than 24 hours later. Dose metrics were recorded for both procedures, no comments were made, and while the skin dose for a single procedure was likely insufficient to cause a severe skin reaction, the two procedural doses combined resulted in a severe injury to the patient.
In both cases, regulations were in place requiring dose metrics to be recorded, yet neither of the physicians was aware of or commented on the dose. Further, in both cases the involved physicians were radiologists, a specialty that often points to their training in residency and fellowship as indicating that they are well versed in radiation management in fluoroscopy. In fact, in our experience, a radiologist was the performing physician in at least 50% of cases involving a patient skin injury during FGI.
Instead of relying on compliance with regulation to keep patients safe, effort and resources should be focused on establishing a safety culture. This includes appropriate training of all personnel, including technologists, nurses, and providers, on radiation safety and radiation management; writing and regularly updating policies and procedures regarding radiation management, occupational protection, and patient management and follow up; and conducting regular reviews of imaging protocols and procedural radiation doses. This is in keeping with the recommendations of accrediting organizations, such as The Joint Commission (2011).
The lack of broad existing regulations that meet the recommendations proposed by professional societies and standards organizations is not an excuse for failing to implement these recommendations. The cost to a healthcare organization of failing to address these recommendations could be far greater than a Level 1 citation. As seen in Figure 2, radiation skin injury can be an extremely debilitating and morbid long-term complication. Litigation costs not withstanding, a healthcare organization must consider the potential cost of negative publicity from such an incident.
Preventing FGI Injuries
Policies and procedures implementing a comprehensive patient safety program in fluoroscopy are the most important element in preventing FGI injuries. The ideal program would include three phases: pre-procedure, intra-procedure, and post procedure (Steele, Jones, & Ninan, 2012).
The actions described below address only the optimization of an FGI; providers must ensure that all FGI are medically necessary, i.e., justified (NCRP, 2011).
Pre-procedure Phase
• Train providers and staff who use fluoroscopy.
All providers using fluoroscopy should be trained for the type and complexity of procedures they are privileged to perform. Didactic and hands-on training should be integrated into an organization’s privileging process. The report of Task Group 124 of the American Association of Physics in Medicine (AAPM) provides detailed guidelines on this process (2012). In addition, providers and staff involved in FGI, including technologists and nurses, should be educated on radiation safety and their roles in the patient safety program. Several excellent commercial training programs are available that follow the AAPM recommendations. The AAPM maintains an updated list of these programs in its Educators Resource Guide.
• Perform informed consent.
The informed consent process for potentially high-dose FGI should include informing the patient about the small risk of a radiation-induced skin reaction and the procedures in place to prevent such reactions (Miller et al., 2003).
• Identify patients at increased risk for skin injury.
Certain pre-existing conditions and medications are known to render patients more susceptible to radiation-induced skin reactions. The most important of these are obesity, prior irradiation of the same skin site, and diabetes (Koenig, Wolff, Mettler, & Wagner, 2001). Particular attention should be paid to the safe use of fluoroscopy during FGI performed on such patients.
• Prepare for special cases including pediatric and pregnant patients.
Specific actions should be taken to manage dose during procedures performed on pediatric and pregnant patients. A convenient checklist of these actions can be found online (Fluoroscopic Safety, LLC).
Intra-procedure Phase
• Implement notification levels.
Organizations should have policies implementing notification levels (NCRP, 2011), typically reference air kerma thresholds at which the operator and managing physician are notified about the radiation dose used thus far during the procedure. Notification levels may be associated with specific recommendations, e.g., to ensure that good practice is being used to minimize the radiation dose rate (Steele et al., 2012).
• Reduce dose rate imaging protocols for special cases.
Tools should be available to help the operator select the appropriate radiation dose rate for different patients and clinical tasks. This might include specific imaging protocols for pediatric patients and adult imaging protocols at low, normal, and high dose rates.
• Calibrate dose monitoring devices.
A qualified medical physicist should, as part of the annual performance evaluation of all interventional fluoroscopes, assess the accuracy of the calibration of the integrated dose-measuring system. This is especially important for notification levels, as regulation requires only that the displayed reference air kerma is within +/- 35% of the true. The measured calibration factor should at a minimum be factored into notification levels and be programmed into the fluoroscope if possible.
• Maintain situational awareness
The operator, managing physician, and staff involved in FGI should be aware at all times of the total radiation dose used at any point during an FGI and the current radiation dose rate. Radiation dose should be managed using the same techniques as used for iodine contrast.
Post-procedure Phase
• Record and review dose information.
Fluoroscopy dose metrics—including but not limited to fluoroscopy time, kerma area product, and reference air karma—should be recorded for each procedure and reviewed on a regular basis. Facility data should be organized into facility data sets (FDS) (Balter et al., 2011), which should be compared to advisory data sets (ADS) such as the RAD-IR study (Miller et al., 2003).
• Set a substantial radiation dose level.
Organizations should establish a Substantial Radiation Dose Level (SRDL) for FGI. The SRDL is the level of a dose metric, preferably reference air kerma, that triggers the organization’s patient follow-up process when exceeded. NCRP 168 recommends 5 Gy reference air kerma as a starting point for the SRDL (2011).
• Establish policies and procedures for patient follow-up after cases in which SRDL is exceeded.
The patient follow-up process should include notifying the patient that the SRDL was exceeded and why, providing simple instructions for the patient, scheduling a 4 week in-person or telephone follow-up, and establishing a referral relationship with a radiation oncologist for management of suspected skin reactions (Steele et al., 2012).
• Record necessary information for estimating the peak skin dose.
Information necessary for estimating the peak skin dose (PSD) from the reference air kerma should be recorded for all procedures during which the SRDL is exceeded. At a minimum, this should include the patient table height during the procedure and would ideally include gantry angles for all acquired images. It is important to measure the height of the table before lowering it to hold compression on the access site or to transfer the patient.
• Manage suspected skin reactions.
All skin reactions following FGI should be considered radiogenic until proven otherwise. Radiation oncologists are typically the clinicians most experienced in managing radiation skin reactions, however, they do not usually see the types of single-fraction doses that can be delivered during FGI. Management of the patient is the responsibility of the physician performing the FGI until complete resolution of any skin reaction is achieved. After extremely large doses of radiation (e.g., > 15 Gy), interim healing may be observed followed by ulceration, breakdown, or necrosis of the affected skin site. Keeping the skin intact is of utmost importance. Severe injuries may require surgical intervention and may never heal completely.
Recommendations for Patients and Referring Providers
Several years ago, the first news articles detailing radiation-induced skin reactions resulting from inappropriate radiation exposures during CT brain perfusion studies received national coverage (Bogdanich, 2010). As a result, patients became acutely aware of concerns regarding the use of radiation in medical imaging and now frequently ask questions about radiation dose when their physician places an order for a CT scan. However, most patients remain completely unaware of the potential radiation risks from FGI. This is at least partially attributable to the number of medical disciplines performing FGI for the diagnosis and treatment of disease.
Referring providers are key in providing information to help patients understand the potential benefits, risks, and alternatives of the procedure they are considering. Therefore, educating referring providers on the potential risks of FGI is essential. While it is not necessary for referring providers to understand the detailed concepts of radiation management and patient safety in fluoroscopy, it is useful for them to possess general knowledge of the potential risks of FGI, which FGI are potentially high-dose, and patient-specific risks factors (Miller et al., 2003). Recent articles including a review of radiation effects on patients’ skin and hair fill this gap nicely (Balter et al., 2010).
With basic knowledge in hand, referring physicians will be able to inform their patients that an FGI will expose them to radiation and offer a complete picture of the benefits and risks of the procedure being considered. These providers can also take the next step and inquire if the specialists to whom they refer their patients have completed formal training on radiation management and the safe use of fluoroscopy. By doing so, they are not only looking out for the best interests of their patients but are also insisting on a level of safety beyond that of most providers.
A. Kyle Jones earned his BS in physics from Furman University and his MS and PhD in medical physics from the University of Florida. Jones is currently employed as a diagnostic medical physicist and assistant professor at MD Anderson Cancer Center in Houston, Texas. He may be contacted at kyle.jones@mdanderson.org.
Alexander Pasciak earned his BS in electrical engineering from the University of Washington and his MSc in health physics and PhD in nuclear engineering from Texas A&M University. Pasciak is currently employed as diagnostic medical physicist and associate professor at the University of Tennessee in Knoxville and may be contacted at alexander.pasciak@gmail.com.
References
American Association of Physicists in Medicine. (n.d.). Educators Resource Guide. Retrieved from https://www.aapm.org/education/ERG/FLUORO/
American Association of Physicists in Medicine. (2012). A guide for establishing a credentialing and privileging program for users of fluoroscopic equipment in healthcare organizations. Report of AAPM Task Group 124.
Balter, S., Hopewell, J. W., Miller, D. L., Wagner, L. K., & Zelefsky, M. J. (2010). Fluoroscopically guided interventional procedures: A review of radiation effects on patients’ skin and hair. Radiology, 254, 326–341.
Balter, S., Rosenstein, M., Miller, D. L., Schueler, B., & Spelic, D. (2011). Patient radiation dose audits for fluoroscopically guided interventional procedures. Medical Physics, 38, 1611–1618.
Bogdanich, W. (2010, July 31). After stroke scans, patients face serious health risks. The New York Times. Retrieved from http://www.nytimes.com/2010/08/01/health/01radiation.html
Center for Devices and Radiological Health. United States Food and Drug Administration. (1994). Public Health Advisory: Avoidance of serious x-ray induced skin injuries to patients during fluoroscopically-guided procedures. Retrieved from http://www.fda.gov/MedicalDevices/Safety/AlertsandNotices/PublicHealthNotifications/ucm063084.htm and http://www.fda.gov/downloads/Radiation-EmittingProducts/RadiationEmittingProductsandProcedures/MedicalImaging/MedicalX-Rays/ucm116677.pdf
Daniel, J. (1896). The X-rays. Science, 3, 562-563.
De Olazo Banaag, L., & Carter, M. J. (2008). Radionecrosis induced by cardiac imaging procedures: A case study of a 66-year-old diabetic male with several comorbidities. Journal of Invasive Cardiology, 20, E233–E236.
Fluoroscopic Safety, LLC. Checklists for Pediatric and Pregnant Patients. Retrieved from http://fluorosafety.com/Pediatric_patient_checklist.pdf and http://fluorosafety.com/Pregnant_patient_checklist.pdf
Henry, M. F., Maender, J. L., Shen, Y., et al. (2009). Fluoroscopy-induced chronic radiation dermatitis: A report of three cases. Dermatology Online Journal, 15, 354–358.
Koenig, T. R., Wolff, D., Mettler, F. A., & Wagner, L. K. (2001). Skin injuries from fluoroscopically guided procedures: Part 1, Characteristics of radiation injury.” American Journal of Roentgenology, 177, 3–11.
Koenig, T. R., Mettler, F. A., & Wagner, L. K. (2001). Skin injuries from fluoroscopically guided procedures: part 2, review of 73 cases and recommendations for minimizing dose delivered to patient. American Journal of Roentgenology, 177, 13–20.
Miller, D. L., Balter, S., Cole, P. E., Lu, H. T., Schueler, B. A., Geisinger, M., et al. (2003). Radiation doses in interventional radiology procedures: The RAD-IR study. Part I: Overall measures of dose. Journal of Vascular and Interventional Radiology, 14, 711–727.
National Council on Radiation Protection and Measurements. (2011). Radiation dose management for fluoroscopically-guided interventional medical procedures. NCRP Report No. 168.
National Council on Radiation Protection and Measurements. (2014). Outline of administrative policies for quality assurance and peer review of tissue reactions associated with fluoroscopically-guided interventions. NCRP Statement No. 11.
Shope, T. B. (1996). Radiation-induced skin injuries from fluoroscopy. Radiographics, 16, 1195–9.
Steele, J. R., Jones, A. K., & Ninan, E. P. (2012). Quality initiatives: Establishing an interventional radiology patient radiation safety program. Radiographics, 32, 277–287.
The Joint Commission. (2011). Radiation risks of diagnostic imaging. Sentinel Event Alert, 47. Retrieved from http://www.jointcommission.org/sea_issue_47/
Ukisu, R., Kushihashi, T., & Soh, I. (2009). Skin injuries caused by fluoroscopically guided interventional procedures: Case-based review and self-assessment module. American Journal of Roentgenology, 193, S59–S69.
