Using Data Analytics to Change Behavior
By Nicole Karchner, PharmD
Data-driven initiative helps increase nurses’ engagement in smart pump safety improvement
The data-analytics application works in conjunction with the smart pump system to create a continuous quality loop to strengthen patient safety, opportunities for improvement, and data-driven insights.
The introduction of “smart pumps” 15 years ago began a new era in IV medication safety. Many of the medications infused directly into a patient’s bloodstream (sedatives, insulin, anticoagulants, opioids) pose a high risk of patient harm; in fact, IV medication errors are twice as likely to cause patient harm compared to medications delivered via other routes (American Society of Health-System Pharmacists, 2008). A simple mistake in programming a pump—pressing “603” instead of “6.3,” or “25,000” instead of “2,500”—can deliver a massive, even fatal, overdose. With smart pumps, if infusion programming exceeds hospital-established limits, the dose-error-reduction software (DERS) generates an alert that must be addressed before infusion can begin. By using the safety features on smart infusion pumps, nurses can help improve patient safety and avert the medication errors associated with the greatest risk of harm: IV administration errors at the point of care (Wilson & Sullivan, 2004; Williams & Maddox, 2005; Fields & Peterman, 2005; Maddox, Danello, Williams, & Fields, 2008).
In addition to providing DERS, smart pumps also automatically capture previously unavailable data on IV infusions. An advanced data-analytics applicationa allows staff to more readily view, report, and use these data to identify key areas for improvement, without the burden and expense of additional staff, software, or daily data management. Staff can take actionable items such as necessary revisions to the DERS drug library, use their expertise to make the needed changes, and then implement the revised dataset hospitalwide in a continuous quality feedback loop.
Orange Regional Medical Center (ORMC) in Middletown, New York, is a 383-bed, Joint Commission–accredited hospital and member of the Greater Hudson Valley Health System (GHVHS). ORMC implemented smart pumpsa in 2005, followed by computerized prescriber order entry (CPOE) and barcode medication administration (BCMA) in 2011; it began regular use of the smart pump data-analytics applicationb in 2015. 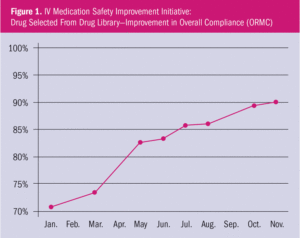
Except for rare instances such as clinical emergencies or investigational drugs, nurses at ORMC are expected to use DERS for every IV infusion. Studies have revealed less valid reasons for not using DERS: underappreciation of risk, a failure to adjust the drug library when alerts are not credible, and a culture that tolerates at-risk workarounds (Institute for Safe Medication Practices, 2007).
Like many hospitals, ORMC found eliminating workarounds to be challenging. Despite extensive efforts, nurses continued to use the DERS drug-dosing safeguards for only 70%–75% of infusions. Then, in 2015, ORMC launched an innovative, data-driven IV Medication Safety Improvement Initiative that increased nursing compliance with the use of the DERS drug library for selection of the medication to be infused (Figure 1). Improved communications and advanced data analytics were keys to success.
This article includes a brief description of the IV Medication Safety Improvement initiative, the remotely hosted data-analytics application, and lessons learned for increasing pharmacy-nursing collaboration, optimizing the drug library, and improving smart pump drug-selection compliance and IV medication safety.

