Transforming Practice with Mobile Clinical Tools: How UCLA Medical Center Specialists Developed and Launched an Innovative Clinical Computing Solution
January / February 2007
![]()
Transforming Practice with Mobile Clinical Tools
How UCLA Medical Center Specialists Developed and Launched an Innovative Clinical Computing Solution

Like their colleagues everywhere, neurosurgeons at Los Angeles’ prestigious UCLA Medical Center struggled until recently with classic problems of availability and usability of clinical data. For one thing, these specialists require a great deal of up-to-date clinical information from multiple data sources.
“As a matter of day-to-day practice, we neurosurgeons work with neurology, neuropathology, oncology, pulmonary specialists from the ICU, and other specialists in planning treatment and care for our patients,” explained Neil Martin, M.D., chief of UCLA Medical Center’s Division of Neurosurgery and professor at the David Geffen UCLA School of Medicine. “A multidisciplinary approach to the tumors and neurovascular disease we treat every day is essential to how we provide care.”
Yet the data needed by UCLA’s neurosurgeons to make good clinical decisions was never timely or useful enough. Not surprisingly, Dr. Martin expressed immediate interest when he learned that a few of his physician colleagues had begun collaborating with UCLA’s Brain Monitoring and Modeling Lab to develop the ability to continuously view EEG (electroencephalogram) results on mobile handhelds and other devices. An initial version of that capability came online as early as 1999. Soon, Dr. Martin was leading an IT development effort within his department that would result in the ability to display near real-time data on a critically ill patient — all in one place and on one computer screen. That leadership helped spawn all the following developments.
Meanwhile, attending physicians from all specialties were expressing the desire to be able remotely (from home and elsewhere) to view patients’ current vital signs data, lab results, medication lists, and other key clinical data, as patients underwent surgery, awaited care in the hospital’s emergency room, or were treated in the ICU.
What began as a project to help neurosurgeons access the most recent and useful data to treat patients evolved into a broader information technology initiative at UCLA Medical Center. Eventually, that effort was commercialized in 2005 as a separate IT company called Global Care Quest (GCQ). Headquartered in nearby Aliso Viejo, and with UCLA as the firm’s alpha development site and the cradle of its innovations, GCQ’s software suite, ICIS (Integrated Clinical Information System), formally launched at the 2006 HIMSS conference in San Diego.
The development of ICIS addressed a classic problem faced by most hospitals nationwide. Clinicians are forced to deal with disparate data located in unrelated databases that are not integrated or made available as an ensemble, in any coherent or easily usable way. Neurosurgeons, like their colleagues in other medical specialties, need the right information at the right time, and need to be able to access comprehensive, flexible views of data across care settings.
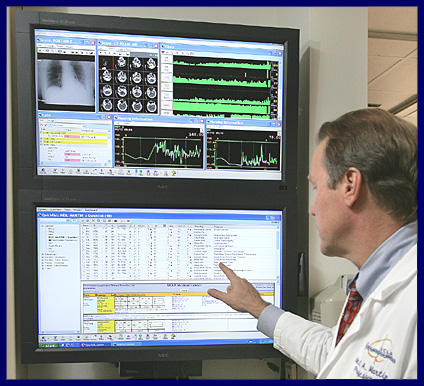
Dr. Martin readily summarized the moment-to-moment needs the ICIS solution was designed to address. “As I move through my day, I’m working in a number of different environments. I’ve got a desktop in my office; but if I’m walking through rounds, I might be using a PDA or a tablet PC. Here, some of our doctors are even using new, very small, ultra-mobile computers, and some are using cell phones. I might be waiting in front of an elevator at the hospital or walking across the street. With ICIS I’ve got the relevant information configured in the appropriate way for the relevant information platform, which could mean for printing out onto paper for rounding, or in some other format. That flexibility of format presentation, combined with the ability to get all the data in one place, is what we are achieving with ICIS.”
Not surprisingly, UCLA’s neurosurgeons, as well as other specialists, have welcomed the use of ICIS. One component of the core solution, which combines views of disparate data on a single screen, is known as ICIS Dashboard, and gives physicians tremendous flexibility as to how they view and use clinical information in real time. Paul Vespa, M.D., director of UCLA’s Neurocritical Care unit, is a firm advocate of the solutions package at the core of ICIS. “The value of this set of tools is quite high, because it serves to organize all the information coming out of the electronic medical record,” Vespa said. “ICIS allows us to query information in a structured way, to trend lab values; and it allows us to create a usable note at the click of a button. Also it helps us organize our thought process about the patient, helping us prepare better care plans based on more up-to-date information. And it helps us to avoid having to generate a lot of the paper-based documentation for billing and reimbursement purposes.”
In a recent visit in his office, Dr. Vespa demonstrated the ease with which he is able to look at his current cases, drawing information from a variety of sources and manipulating the views of that disparate information on the two screens on his desk. Vespa moved from one view to another to a third in a few rapid-fire clicks, showing the visitors why and how he might want one particular view of various data points at one moment and another view of that same data the next moment. “I think this solution easily saves us an hour’s worth of documentation per physician per day,” he said.
What’s more, Vespa noted, “The generation of an organized note that is created in this system serves as a game plan for the whole team — nurses, respiratory care therapists, pharmacists, other physicians, and other physician consultants who come in. And each of those individuals can look at the generated note and really have a game plan for the day. There used to be a time when instead of writing that note, we dictated our notes, and the dictated notes would come back to us six hours later, and would then appear on the EMR. The dictation wasn’t always immediately available, so it couldn’t do any of the coordination; as a result, no one would know exactly what was going on.”
 |
|
| Neil Martin, M.D. Chief of UCLA Medical Center’s Division of Neurosurgery and professor at the David Geffen UCLA School of Medicine. Photo courtesy of Global Care Quest |
According to Vespa, “now the time neurosurgeons save each day by not having to reiterate instructions or repeat information is immeasurable.” And the fact that a neurosurgeon’s note can be quickly and easily passed along strongly enhances that physician’s productivity and effectiveness, as well as all those involved in the chain of clinician communication.
“This is really the first application that’s been able to bring all the relevant information into one view; I like to say it’s the only one that puts that information right there in your face,” Dr. Martin said. “The other EMR applications have configurations similar to Microsoft Word, that require you to understand multiple-tiered menus in order to change views, with no intuitive way of figuring out the various functions. This single-view, at-a-glance, in-your-face, selected-information view is the key advancement we’ve achieved, along with the ability to customize for all the different specialties.”
Different Specialties Find Much to Use
Indeed, physicians in different specialties and clinical environments at UCLA Medical Center are making use of the various elements of GCQ’s solutions, in ways that work for them as members of specialties and as individual practioners. One of the most important uses has been in the intensive care unit (ICU), which went live with GCQ’s rounding list tool in November 2004. The rounding tool uses the same fundamental data as the other elements in the GCQ toolbox, providing up-to-the-minute data on patients in the ICU, streaming that data from various sources in the hospital (laboratory, radiology, pharmacy, monitoring equipment), and allowing the first-year residents who make their clinical rounds every day to quickly gather the key clinical information they need.
 |
|
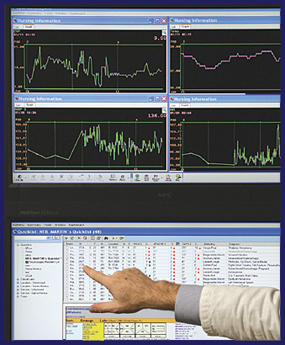
Residents who use the rounding tool say that it has saved them as much as 2 hours a day, a significant savings for everyone involved. Since the implementation of the federal regulation that limits residents’ hours went into effect in July 2003, the availability of resident hours for rounding has been reduced, and every hour of every resident’s time has thus become a more valuable commodity. Within the ICU itself, GCQ created the Data Wall, a graphical dashboard displayed on a 50-inch wall-mounted plasma screen that can fit eight of the mobile displays on a single screen, including individual physicians’ QuickLists, laboratory results, text reports, two x-ray windows, note writing, and a live EKG. Such all-on-one-screen data availability has proven useful to residents and attendings alike.
Meanwhile, another dramatic success has taken place in the area of emergency stroke management. David Liebeskind, M.D., the neurologist who runs UCLA Medical Center’s stroke management programs, says the ability to instantly access key clinical data — and images — from anywhere, is absolutely critical to successful stroke management. “Time to treatment is critical in this area, probably more so than in any other area, including heart attack, ” said Dr. Liebeskind. “And it’s not just time itself that’s important, but getting as much information as possible in a short time, is crucial in stroke treatment. Often, you get very little information, such as, ‘weakness on the right side.'”
In fact, ICIS has been incorporated into a very important clinical initiative at UCLA Medical Center, the first pre-hospital stroke study in the United States, according to Dr. Liebeskind. “We get called on our pagers by paramedics in the field” responding to situations involving apparent stroke onset. “At present, the communication takes place on the telephone, but soon we are going to be implementing video links,” he said.
A key element in this tele-stroke program is the ability of Dr. Liebeskind and his colleagues to instantly access vital data on the patients’ status. For example, getting a diagnostic image on a screen (whether desktop or PDA) to the attending physician handling the emergent case. Gathering past diagnostic images and patient information, and being able to immediately view an MRI brain scan, for example, are critical to the optimal treatment of a patient with apparent emergent stroke symptoms.
Rapid Response Through Mobile Technology
Using the ICIS solution, Dr. Liebeskind and his neurologist colleagues are able to instantly and accurately view diagnostic images anywhere, expanding their clinical capability considerably. Dr. Liebeskind noted that he has successfully consulted on emergency cases while on a ski lift in Taos, New Mexico, hundreds of miles away from UCLA Medical Center. Intervening through case management in a tele-stroke program, he said, “means providing critical information in a crucial timeframe — and sometimes that timeframe lasts no more than a few minutes. Case management is often very quick as a process — sometimes it involves ruling in or ruling out certain factors, very quickly — but if you don’t have critical information available at the crucial moment, including imaging, your role as a stroke neurologist is defeated.”
 |
|
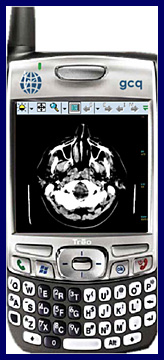
| Brain CT seen in ICIS Mobile’s PACS Viewer Photo courtesy of Global Care Quest |
And while it’s primarily diagnostic images that neurologists like Dr. Liebeskind are looking for in stroke management, nephrologists like H. Albin Gritsch, M.D., find the trending capabilities of the ICIS solution package the most useful.
Dr. Gritsch leads the renal transplantation unit at UCLA Medical Center and noted that the solution “integrates a lot of different systems into one platform, so you don’t have to keep going from one server to the next. The other feature I like a lot is the graphing capability; that capability very quickly allows you to graph lab results and therefore get a trend, which is very important for kidney transplantation.” This is especially true, he said, in trending creatinine levels, a measure of kidney function. Having to move from one computer workstation to another, as he and his colleagues did in the past, was very inconvenient and challenging. Now, Dr. Gritsch said, he’s able to quickly access trend-worthy patient data on his PC or PDA, when he is at home or a satellite clinic, and able to communicate vital information to other clinicians.
Physician Adoption by Word-of-Mouth Marketing
Not surprisingly, as physicians in neurosurgery, neurology, nephrology, the ICU, and other departments at UCLA Medical Center have learned of the benefits of ICIS, more and more have become active users, even with no mandate from hospital management. Indeed, of the 4,600 members of the medical staff at UCLA, nearly 1,500 have registered to use the GCQ system’s tools to date. At the same time, the innovation that has taken place at UCLA Medical Center is spreading, as several other hospital organizations in Southern California have begun implementing the GCQ commercial solution to suit their diverse clinical computing needs.
The diversity of uses to which this toolbox of solutions could be applied doesn’t surprise Dr. Martin. “Initially we just wanted to provide mobile access to the EMR and enhance clinical decision-making and workflow for neurosurgeons and other specialists,” he said. What became apparent very quickly was the need to identify what types of clinical data were mission-critical for physicians, and how to integrate disparate data fields on a single screen and to optimize speed, connectivity, and mobility. The work that began at UCLA, he believes, will be important for all types of hospital organizations, including teaching hospitals, community hospitals, pediatric hospitals, and other types of institutions. Dr. Martin reports, “When I meet people from community hospitals, they cite the same kinds of challenges we’ve faced here.”
Integration, availability, mobility, and shareability of clinical data and information are all themes that make UCLA Medical Center’s IT saga universal for all hospitals as clinical computing continues to evolve. As software solutions like ICIS become more available on the healthcare IT market, more physicians like UCLA Medical Center’s specialists will innovate their care management in the next decade — to the benefit of patients nationwide.
