EMPSF: The Role of Nurse Leaders in Quality and Patient Safety
January/February 2013
![]()
EMPSF
The Role of Nurse Leaders in Quality and Patient Safety
In October 2010, The Institute of Medicine (IOM) released The Future of Nursing: Leading Change, Advancing Health. This report was the result of a 2-year initiative by The Robert Wood Johnson Foundation (RWJF) and the IOM, designed to respond to the need to assess and transform the nursing profession. The report outlines four key messages:
- Nurses should practice to the full extent of their education and training.
- Nurses should achieve higher levels of education and training through an improved education system that promotes seamless academic progression.
- Nurses should be full partners, with physicians and other healthcare professionals, in redesigning healthcare in the United States.
- Effective workforce planning and policy making require better data collection and information infrastructure.
While each of these key messages is important, the last two stand out in light of the nurse executive’s role in promoting organizational quality and patient safety initiatives. These key messages speak to the need to transform the nursing profession in three crucial areas: practice, education, and leadership. They also highlight the need to collect meaningful real-time data on the healthcare workforce and quality indicators to inform planning for necessary changes to the nursing profession and the overall healthcare system.
Nurses Drive Change in Patient Safety Improvements
Quality Defined
Quality is defined in a variety of ways: a peculiar and essential character; an inherent feature; and a distinguishing attribute (Merriam Webster Dictionary). Other definitions include: a degree of excellence (Dictionary.com), the standard of something as measured against other things of a similar kind (Oxford), or a state of being free of deficits, defects and variations of any kind (BusinessDictionary.com). As healthcare focuses on an increasing number of safety initiatives, nurse leaders are key to successful outcomes. But how are these quality initiatives and outcomes defined? How do we best align quality and patient safety? With a myriad of healthcare professionals at the table, nurse leaders must have the skills to set the table for success.
In 2001, the IOM, published Crossing the Quality Chasm: A New Health System for the 21st Century. In this report, quality was described in six dimensions: safe, effective, efficient, equitable, timely, and patient centered. Most definitions have a bit of subjectivity in them and leave room for interpretation, but without a concrete definition it is difficult to set standards, measure progress, and assign accountabilities. Incorporating the six dimensions of the IOM report helps to ensure that the care we provide and the protocols we develop align quality with patient safety for optimal outcomes. This is where exemplary nurse leaders step forward and align teams to lead the development of definitions, outcome measures, and innovative change.
Transforming Quality and Safety Across the Organization
When most nurses enter nursing school, their primary focus is to understand how to care for and respond to the needs of patients, organize a plan of care, and provide ongoing assessment and evaluations of their care. Most do not think of becoming a leader, transforming teams and leading change across a complex system. While there are leadership courses in most nursing school curricula, they do not adequately address the realities of the complexities of the healthcare system, idiosyncrasies of health policy as it unfolds in the clinical setting, or challenges of technology. On top of that, most nurses are concentrating on the clinical arena, understanding pathophysiology, the patient response to illness, and juggling the ever-changing world of pharmacology. They are not ready for the challenges posed by these dynamic organizational systems. This leaves the organizations with the task of educating and grooming future nurse leaders.
While the role of nurse leaders is important, healthcare experts encourage all members of the interprofessional team to understand organizational dynamics to enable better integration and implementation of change to improve outcomes. Research and evidence-based practice continue to identify the importance of collaborative and diverse teams. Nurse leaders are well positioned in the organization to lead and partner with other members of the interprofessional team.
Strategies that dynamic and respected nurse leaders use must be creative and innovative. Some key strategies are to be visible on the clinical units, communicate effectively the importance of a patient-centric environment, and share their vision for excellence. They should also engage in active and visible partnerships with physician colleagues. This partnership should start at the CNO/CMO level and continue to the individual unit level. This model has been successful at the University of Pennsylvania Health System. Most units use a partnership entitled Unit-Based Clinical Leadership (UBCL) teams that consist of physician, nurse, and quality experts as team leaders for a diverse and dynamic interprofessional team (Figure 1). Some of the projects they have undertaken include: reducing the left-without-being-seen (LWBS) rate in the emergency department; multidisciplinary rounding; discharge education; and patient- and family-centered care. These projects align with the University of Pennsylvania Health System Blueprint for Quality and Patient Safety.
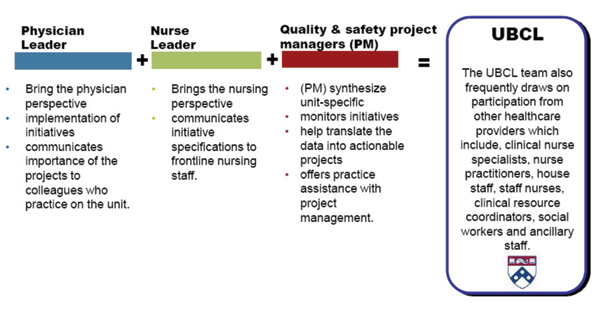
Figure 1. Unit-Based Clinical Leadership (UBCL) Model.
It is essential that nurse leaders of the future have the right combination of clinical acumen and organizational awareness. They must be able to build strong and collaborative interprofessional partnerships and lead complex change. Their leadership style should promote interprofessional collaboration, transform the team, inspire them to want to do more, and support innovative ideas. This requires a great deal of courage and determination. Nurse leaders must recognize that quality and patient safety cannot be dictated from the top. It is an overarching culture that needs to be cultivated and nurtured so that all members of the team understand the importance and significance. Nurse leaders who can role-model excellence, clear communication, collaboration, and courage help bring teams into alignment and ensure the best possible outcomes for the organization, the teams, and most of all, our patients.
AnnMarie Papa is clinical director of emergency and observation nursing at the Hospital of the University of Pennsylvania & Penn Presbyterian Medical Center and 2011 President of the Emergency Nurses Association. She may be contacted at ampapa108@hotmail.com.
Victoria Rich is chief nurse executive and associate executive director at the Hospital of the University of Pennsylvania and assistant dean of clinical practice at the University of Pennsylvania School of Nursing. She may be contacted at victoria.rich@uphs.upenn.edu.

The Emergency Medicine Patient Safety Foundation sponsors this column. For more information, visit www.empsf.org.
