The Return on Investing in Elder Care
Business case for age-friendly health systems offers push to standardize best practices
By Megan Headley
By 2030, every one of the 78 million baby boomers will be over 65, reports the U.S. Census Bureau, a figure that will exceed the number of children for the first time in history. These are staggering statistics, and to effectively care for all these aging adults, providers must implement solutions today.
While healthcare providers are aware of these statistics, and many health systems are already hitting upon effective solutions to care for older adults, there’s an overall lack of consistency in how systems approach this challenge.
That’s what the Institute for Healthcare Improvement (IHI) is trying to change.

A framework for elder care
“We have a growing number of older adults in the system,” says Leslie Pelton, MPA, senior director for IHI. “We know that they are harmed more often by the system, and we also know that their care can be quite complex. We also know how to take care of those adults really, really well. That’s the 4Ms.”
The 4Ms are the framework that emerged from IHI’s Age-Friendly Health Systems initiative, launched together with the John A. Hartford Foundation, the American Hospital Association, and the Catholic Health Association of the United States in 2016.
IHI describes an age-friendly health system as one where older adults get the best care possible, experience no healthcare-related harms, and are satisfied with the care they receive. These systems are optimized for all participants in this process, including families and caregivers. Achieving these goals is based on meeting four elements that make up the 4Ms framework:
> What Matters: Align care across settings and in accordance with each older adult’s health outcome goals and care preferences, including but not limited to end-of-life care.
> Medication: If medication is necessary, use age-friendly medication that does not interfere with What Matters to the older adult, Mobility, or Mentation across settings of care.
> Mentation: Prevent, identify, treat, and manage dementia, depression, and delirium across care settings.
> Mobility: Ensure that older adults move safely every day to maintain function and do What Matters.
The 4Ms do not introduce a new way of delivering care; rather, they standardize best practices to ensure care is consistently high-quality. As Pelton puts it, the framework is “about moving from the evidence-based care happening sometimes, with some older adults in some places some days, to the reliable practice of the evidence-based care.”
The business case for age-friendly care
In driving adoption of the 4Ms framework, IHI observed that a piece was missing to get more health systems to create a framework for the processes they already were putting in place.
“As the 4Ms emerged and there was more and more interest in adopting those in health systems across the country, we recognized that the places that the 4Ms were in practice weren’t necessarily articulating the business case for doing so,” Pelton says. As she puts it, there are two perspectives that must come together: the clinical care perspective and the business perspective.
This year IHI published a report titled The Business Case for Becoming an Age-Friendly Health System and introduced a return on investment (ROI) calculator that can help health systems form their own business case perspective for adoption of the 4Ms.
As the report explains it, “Making the business case means providing evidence regarding financial returns—the instrumental value—from investing in becoming an age-friendly health system. The business case does not include improved outcomes or satisfaction—the intrinsic value—that result for patients and their families. If the age-friendly health system can show instrumental value, however, its intrinsic value is more likely to be sustained.”
Value has become central to every discussion in today’s healthcare environment. With the cost of healthcare rising to 17.9% of the U.S. GDP in 2017, health systems are cracking down on balancing lifesaving practices with the cost of implementation.
So, IHI set out to develop an ROI calculator that would enable health systems to look at the financial impact of reliably practicing evidence-based care. IHI director Victor Tabbush, PhD, adjunct professor emeritus at the UCLA Anderson School of Management, was recruited to develop a spreadsheet that systems can download to run their own calculations. That tool is now available at IHI.org/agefriendly.
Perhaps not surprisingly, the evidence seems to indicate that reliable evidence-based care is all-around good.

Hartford Hospital tracks the data
Hartford Hospital, an 850-bed inner-city teaching Level I trauma center and one of seven hospitals within the Hartford Healthcare Network, is an example of how a standardized approach can make a strong business case for implementation. The hospital’s approach to screening for delirium is a case study within the new IHI report.
Since 1990, the hospital has had a team of geriatricians and nurse practitioners within its Division of Geriatric Medicine and Gerontology who provide care to seniors in the acute care hospital, sub-acute, long-term, and community settings. The inpatient geriatric consult service, comprised of a geriatrician and an advanced practice registered nurse certified in geriatrics, was frequently asked to see older adults with impaired mental status, fall risk, and frailty; providers and nurses sought help with understanding these patients’ problems and guidance on how to care for them.
“Many of these patients were experiencing delirium and required a more thorough workup to explain the etiology of the delirium and a comprehensive plan of care to keep them safe and cognitively and functionally engaged,” explains Christine M. Waszynski, DNP, APRN, GNP-BC, with Hartford Hospital. “Delirium prevention, treatment, and management were identified by our team as an area in which improvements could be made.”
The hospital’s geriatrics team developed a plan to implement a comprehensive, standardized, and evidence-based delirium program. First, they developed inpatient geriatric consult service team members as true delirium experts. Next, they set out to justify the need to pay attention to delirium by establishing a baseline measurement of delirium prevalence.
A retrospective review of 596 randomly selected patient records from January 1, 2002 to December 31, 2005 found 36.9% of patients experienced delirium during their hospitalization. Moreover, 87.5% of patients who died had experienced delirium at some point during their hospitalization, and 70% of patients who died met criteria for delirium at the time of death. “The collection of data enabled us to demonstrate delirium to be a common syndrome for our patients associated with poor outcomes,” Waszynski explains.
But Hartford Hospital still had gaps to address before turning the numbers around. At that point, there was no formal screening tool in place to assess for delirium, and there was no standardized order set to guide the diagnostic workup and care of these patients. That had changed by 2006, when nursing staff pilot-tested a delirium screening tool that ultimately was rolled out to all units and all patients.
More data supported the corrective actions taken. “As we went to the electronic medical record in 2010, we were able to quantify delirium rates and related outcomes. As we shared this information with hospital leadership, it became evident that delirium prevention and evidence-based treatment and management strategies should be a priority,” Waszynski says.
In 2011, Hartford Hospital launched its Actions for Delirium Assessment Prevention and Treatment (ADAPT) program to screen all patients for delirium, treat those that showed signs, and manage cases that could not be resolved.
An interprofessional team set out to create a pathway for clinicians to work with patients at high risk for or already experiencing delirium. “This team has continued to meet over time to refine our approach based upon new evidence and to review our impact. Our unit geriatric resource nurses play a critical role in the day-to-day oversight of delirium care,” Waszynski says.
Demonstrated cost and care improvement
The time spent managing cases related to delirium was staggering. In 2018, the hospital diagnosed delirium ranging between 5% and 50% of all hospitalized patients within ADAPT-participating units. And that time was associated with incredibly high costs. For example, the hospital spent $96 million in care related to delirium from July 2015 to June 2016 alone.
As the IHI report notes, “While the financial dimension is generally not the decisive factor for adopting the 4Ms, an attractive ROI should serve to encourage the scale-up and spread of age-friendly hospital care.”
Certainly, that was the case for Hartford Hospital. “Leadership of healthcare organizations need evidence to determine where resources should be prioritized in order to better service their patient population,” Waszynski points out.
According to Dr. Robert Dicks, Hartford Hospital’s geriatrics program director, “It is optimal to demonstrate not only the projected cost saving but the actual impact of a program using your own data. Real-time data allows for feedback, quality assurance, and the engagement of clinicians and leadership.”
Prior to running the numbers through IHI’s ROI calculator for age-friendly health systems, Hartford Hospital tracked its own ROI across several criteria through a delirium registry that captures the hospital’s delirium prevalence and incidence with related outcomes.
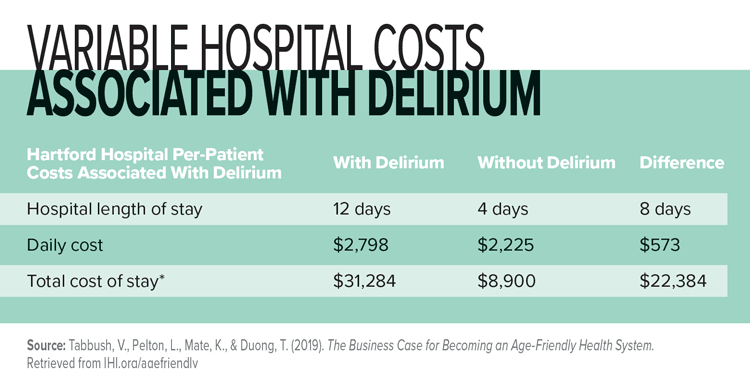
With the assistance of ADAPT team members of the Hartford HealthCare Research Institute, that data has demonstrated a 40% cumulative decrease with an incremental 8% decrease annually in delirium-attributable days—without an increase in hospital mortality or readmission in patients developing delirium. The team also has demonstrated a decrease in 30-day readmission rates and an increase in return-to-home transition at time of hospital discharge for this vulnerable population. “This was accomplished in spite of increased acuity and census,” Waszynski adds.
And the business case? Waszynski says, “We found that the number on the calculator was very close to the number we had calculated ourselves: $6 million in savings annually from the ADAPT program.”
ADAPT screened more than 31,000 patients at Hartford Hospital in 2018. Plans are in process to replicate ADAPT across the system’s hospitals, starting with a demonstration project in one setting. Components of ADAPT have been implemented in postacute settings with an ongoing evaluation of the impact.
Adding to the evidence
Health systems understand the impact of tying the business case to clinical care. On a recent call introducing the ADAPT program, more than 50 health systems asked questions about how to use the ROI calculator to build their own business case for being an age-friendly health system. These systems have the tools in place but haven’t yet quantified their usefulness.
Pelton also sees this ROI calculator as a way of empowering champions of older adults. “It allows them to make sure they can articulate the business case side by side with the right clinical care for older adults,” she says.
For health systems pulled in so many directions, it pays to understand what actions can be taken to reduce costs—and to apply that funding to broader ways of providing safe, quality care.
Megan Headley is a freelance writer and owner of ClearStory Publications. She has covered healthcare safety and operations for numerous publications. Headley can be reached at megan@clearstorypublications.com.
