Sound the Alarm
By Leah M. Addis, MA, CPASRM; Vladimir N. Cadet, MPH.; and Kelly C. Graham, BS, RN
How much noise is heard over the course of the day in the average hospital unit? One study found alarm rates up to 700 per bed per day (ECRI Institute, 2013a; Graham & Cvach, 2010). When alarms sound so frequently, they simply cannot be managed adequately. Ineffective alarms lead to alarm fatigue among staff members, increased risk of patient harm due to an unanswered alarm, and dissatisfaction among both patients and staff with the hospital environment (ECRI Institute, 2013b).
A review of events seen by ECRI Institute Patient Safety Organization (PSO) highlights many common alarm sources. For example, these alarm-related event reports frequently involved physiologic monitors, ventilators, intravenous pumps, bed alarms, and chair alarms. Upon further review, it was found that additional alarms such as those from tube-feeding pumps, infant security systems, intra-aortic balloon pumps, medical gas systems, and even fire alarm systems were being reported as well. The amount of clinical alarms that hospital staff hear, process, and manage quickly becomes very significant; when non-medical equipment alarms are considered as well, the overall noise level within a facility can become overwhelming.
Common themes identified across the event reports reviewed include:
- Alarms that did not sound, due to either user error or equipment issues
- Alarms that were not promptly addressed, mainly physiologic alarms
- Alarm-related miscommunication, such as a misunderstanding about who was supposed to respond to the alarm, or a lack of notification to the clinician that an alarm was occurring
It is no surprise to ECRI Institute that this issue has been recognized by The Joint Commission and other patient safety organizations as one that requires significant attention. Alarm hazards have ranked as one of ECRI Institute’s Top 10 Health Technology Hazards every year since 2007, when the list was first created (ECRI Institute, 2013b). There is no easy answer to the dilemma of how to create an effective alarms management system. Even in the text of the 2014 National Patient Safety Goal, the Joint Commission acknowledges that “universal solutions have yet to be identified” and that “solutions may have to be customized” (Joint Commission, 2013, p. 7). In short, there is no silver bullet.
As healthcare facilities advance through the timeline set by the Joint Commission in its 2014 National Patient Safety Goal, alarm management and safety priorities may seem daunting in scope and execution.
Indeed, by now, hospitals should be working toward the goal of reducing “the harm associated with clinical alarm systems.” The Joint Commission has stipulated that this safety goal should be a facility-wide initiative by July 1, 2014. Also in 2014, an overall risk assessment of clinical alarms should be performed and used to determine the focus of the hospital’s alarm management plan, including selection of which alarms will be addressed. Factors that should be taken into consideration include (Joint Commission, 2013):
- Necessity of the alarm
- Risk if the alarm goes unanswered or fails
- Review of related facility adverse events, current best practices, and guidelines
- Engagement of clinicians
By January 1, 2016, strategies for improving alarm management and decreasing risk, which will have been derived from findings of that initial assessment, need to be established and implemented through the development of updated policies and procedures, as well as staff education regarding the use and management of clinical alarms. New or revised policies should review responsibilities and guidelines for setting, changing, and disabling alarms—including who has permission to do so, when it is permissible to do so, and under what circumstances alarm settings may be changed or disabled—as well as include a clear process for attending to the various alarms and verifying that they are set and functioning appropriately.
Therefore, hospitals need not only to assess their alarm management practices now, but to also begin laying the foundation for a stronger and more comprehensive alarm management program. A task force including representatives from frontline staff, nursing, medical leadership, telemetry, clinical engineering, information technology, patient safety, risk management, and others as appropriate, should be convened to lead the hospital’s alarm program review and revision, (ECRI Institute, 2013b).
Instead of approaching necessary high-level organizational changes as one single obstacle, approaching them from four different perspectives allows the resulting alarm management program to be stronger and more effective.
 |
|
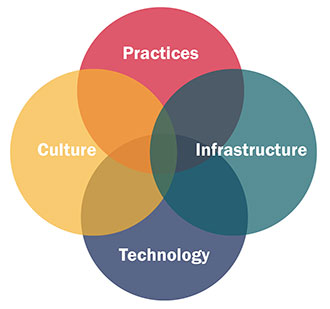
| Figure 1. A Synergistic Approach ECRI Institute’s four alarm management tenets—culture, practices, infrastructure, and technology—all must be incorporated into an alarm management program for it to be most effective. |
ECRI Institute refers to these perspectives as the four tenets of alarm management: culture, infrastructure, practices, and technology. Each presents its own unique challenges when creating an alarm safety strategy, and each offers distinct advantages when it supports an alarms initiative. With that in mind, an alarms self-assessment should include the following steps:
- Assess the organization’s culture.
- Review infrastructure-based capabilities.
- Clarify best practices.
- Maximize technology use.
The Four Tenets of Alarm Safety
Attacking alarms issues from the perspectives of cultural readiness, infrastructural preparedness, best practice application, and technological optimization will produce a stronger initiative for improving alarms safety across the organization. The dynamic relationship of these four tenets can be difficult to address comprehensively. Though the four areas each require individual attention, any alarm management strategy must not dwell too much in any one “silo”; rather, coordination across all fronts of the alarm management initiative should ensure that changes in each of the areas support those in the others (Figure 1).
Culture
First and most importantly, leadership and senior staff members are responsible for modeling the culture of the organization. A culture of safety—in which a systems approach is used to identify process errors, staff are empowered to speak up regarding safety concerns, and teamwork is an obligation (ECRI Institute, 2013b; Paine et al., 2004)—is exemplified by the appropriate actions and conversations at all levels of the organization. This tone is both set and reinforced when it is demonstrated by organization leaders. Staff members look to leadership for guidance regarding patient safety and alarm management policies and procedures, so it is at that high level where alarm management should be understood and modeled as a core value.
Second, fostering an attitude of ownership among staff can stimulate a sense of “all hands on deck” and be used to educate staff members about the immediacy of alarm hazards. Staff “champions” should help fellow staff members understand the seriousness of alarm hazards and should also demonstrate how an effective alarms strategy will reduce nuisance alarms, delayed alarm response, and uncertainty regarding alarm response procedures and protocols. Staff champions can also help other staff members learn how to work with any new technologies as well as how to comply with new policies and procedures.
Education is another component of cultural evolution, as is reinforcement of new alarm management priorities and practices (e.g., alarm coverage, permissions, skills, and competencies for appropriate staff members). Education needs to be consistent—both in message and frequency. Training should be as standardized as possible in order to ensure that all staff members in the hospital have received the same training and can respond appropriately to an alarm regardless of location. Guidance should be made available to staff members regularly and on an as-needed basis.
Scenario #1: The hospital network’s effort to improve frontline staff accountability and empowerment regarding safe alarm management practices includes routine education for all nurses and frontline staff. However, it is inconsistent; education varies from unit to unit as well as for float nurses, not to mention among hospitals within the network. So, when emergency department nurses from a hospital within the system float to one of the telemetry units, they find that electrode replacement practices are different and aren’t sure how to proceed. How can educational practices be improved?
Lessons learned
Clearly, since each unit may require a customized way to handle alarms, it is important to ensure that all nurses understand the standard of practice in the units they are assigned to, especially when floating. Therefore, an education structure should be standardized across the hospital so that all staff members know what to expect, e.g., checklists, mini-orientation, printed materials, no matter which unit they are floating to.
Another strong educational strategy for staff training is simulation exercises. Such practice can help staff members to truly understand the protocols of the unit in which they will be working. The clinicians who determine these protocols and who are responsible for the communication of them need to be involved and engaged in the process as well. For example, in this scenario, simulation-based training should be planned in advance for nurses floating to the unit. Advance planning is prudent because of the time it can take to prepare a simulation and ensure that staff members are able to attend the training. Training should include the importance of daily leads and electrode placement, as well as training on skin integrity assessment. Simulation training in such circumstances helps nursing staff to be engaged. Likewise, training should help staff situate specific unit protocols within organization safety initiatives; in this scenario it should be understood that effective electrode placement can decrease nuisance alarms and reduce the overall alarm load.
Infrastructure
Any discussion of infrastructure should include not only architectural layout but also staffing patterns, care models, and alarm coverage strategies. The layout of the unit should always be considered when reviewing or revising staff workflow and coverage models. When the layout supports the care model, staff members are better able to care effectively for their patients; however, the layout of the unit can also impede workflow and staffing patterns. This is why it is beneficial to consider workflow and staffing patterns when building or remodeling a unit or facility.
Staffing patterns and physical layout will jointly influence the decision to implement a centralized or decentralized alarm coverage structure. For example, will it be more effective within a specific unit to route all alarms to a central “cockpit” or to implement a decentralized model, in which alarms sound either from the source in patient rooms or at local nursing stations?
Policies, procedures, and guidelines should also be assessed as part of a review of organization infrastructure. For example, how will alarm coverage responsibilities be divided?
Scenario #2: The hospital’s alarm management committee decides to institute zones (designated areas), install alarm enunciators (remote speakers) in the hallway, and install hallway monitors (screens that replicate monitor data) in their effort to improve patient monitoring. However, after the hallway monitors were purchased, the walls were found to be structurally incapable of supporting them, and the plan has to be revised. What should have been done?
Lessons learned
Oftentimes, the tendency is to plan for these situations after the need arises. But, it is more efficient to plan for issues well in advance of an installation, in order to head off such unwanted complications. It is prudent to plan proactively rather than reactively. This prevents unnecessary costs or delays due to a second round of purchasing, repairs, or retrofitting.
In this instance, a better strategy would have been to build in lead time for a more extensive planning phase and to include those staff members with relevant responsibilities during the planning phase. For example, facilities staff should have been asked by the alarms committee about the structural capabilities of the walls, as well as National Fire Protection Association (NFPA) codes and standards, as this could affect placement of such monitors. While expanding nurse coverage capabilities and improving response time may require remote monitors, structural concerns need to be addressed first, before the technology is purchased and certainly before it is installed (Cadet, 2014).
Practices
When creating a new alarms management strategy, specific process steps for alarm notification, verification, and response will need to be clarified and communicated. This delineation of responsibility and accountability among all caregiving staff will require support at all levels of the organization. Some processes that will need to be reviewed and clarified as needed include:
- Alarm escalation plans and verification of alarm response: Through what process is the alarm escalated, and how do other staff members know when an alarm has been answered?
- Monitoring and communication regarding patient transport: Who is responsible, for example, for replacing patients’ telemetry leads after they return from an imaging study?
- Admitting patients to and discharging them from telemetry or other physiologic monitoring: What criteria should be observed in making such decisions?
Scenario #3: The hospital was in the process of updating its telemetry guidelines. In the meantime, a patient was admitted and placed on telemetry. This patient was sent for an imaging study, and a staff member was assigned to provide transport to and from the study. When returning from the study, the staff member handed off the patient to another staffer, who was unsure if the patient needed to be placed back on telemetry, and whose responsibility it was to do so.
Lessons learned:
Corrective strategies in this situation are two-pronged, focusing both on policies and communication. Often, in transport, policies don’t clearly outline staff members’ responsibilities, and it can be unclear who is responsible for communicating these policies to transporters. Likewise, what information needs to be communicated among the unit staff, transporting staff member, and imaging department staff? Who is responsible for this? Effective communication requires that all frontline staff are trained on communication policies and procedures. Are staff responsibilities effectively outlined? Are policies clear and easily accessible?
Technology
Obviously, any alarm improvement initiative will need
to include a component on potential alarm sources, including physiologic monitors, telemetry systems, and other clinical alarms. Bed alarms and non-clinical alarms should not be excluded from a review out of hand, as they also contribute to the overall alarm load of the hospital.
During this assessment, the following questions should be asked:
- Are devices and monitors being used as intended?
- Are staff using the technology to the fullest extent of its capabilities?
- Does the technology meet the needs of the staff?
- Are staff members satisfied with the technology?
- Does the technology (for example, an ancillary notification system) interface and integrate smoothly with existing devices and systems?
Specifically, in order to prepare for and meet the National Patient Safety Goal, the functionality and efficacy of the facility’s alarm systems should be assessed; this begins with a review of the organization’s alarm load in order to determine the alarms systems that need to be prioritized.
Consideration should be given to the reason for purchasing a technological aid, such as an ancillary alarm system (which allows clinical alarms to be communicated to clinicians via personal notification devices, such as smartphones). Installation of such a system should take place deliberately and include sufficient planning, preparation, and testing (Figure 2, pg. 44).
Often, the temptation to use technology as a Band-Aid is hard to resist. However, if there is a problem in the current alarm flow, response, or escalation system, a new technology is equally as likely to compound the problem as it is not to.
Therefore, the importance of a thorough review of the organization’s current alarm management strategies, as well as ensuring adequate time and preparation for any technological implementation, cannot be overestimated. As seen in the following scenario, sometimes planning for a new technology can include the determination that a modification to or reinforcement of the current system would better suit the organization’s needs and capabilities.
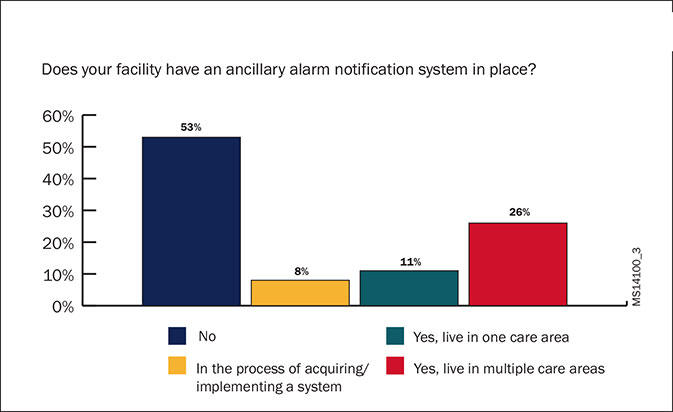
Figure 2. Installation of Ancillary Alarm Notification Systems. A 2013 webinar led by ECRI Institute’s Health Devices found that while just over half of attendees did not have an ancillary alarm management system, just under half either already did install or were in the process of installing such a system. N=321
Scenario #4: The organization purchased an ancillary alarm notification system, but now devices are not integrating smoothly with the middleware (the software that manages data and routes alarms to clinicians’ devices). There is confusion regarding where alarms are originating, the level of alarm, and if alarms have been addressed. How could this have been avoided, and what can the hospital do now?
Lessons learned
Extensive testing should always be part of any technological implementation. Not only will this help to identify and allow time to correct any integration complications, but when testing includes seeking the opinion of potential staff system users, it can act as a barometer of staff interest in the technology. Often, the culture of the organization can indicate staff eagerness as well. How engaged will staff members be with yet another technological device?
Another factor to consider before rushing headlong into an installation is if an upgraded system is even necessary, or feasible. Does the facility have the capacity for an upgraded, integrated alarm system? Determination of current system capabilities and limits is essential before any attempt to install newer systems, which may not be supported by the current wiring (Cadet, 2014). If a system is not implemented well, it could increase risk to the patient via ineffective alarms management.
Moving Forward
Alarms management initiatives are necessarily complex. Creating an effective safety initiative in order to be ready to meet the Joint Commission’s National Patient Safety Goal on clinical alarms takes significant time and planning. Determining and implementing strategies to strengthen each of the four tenets of alarm safety will allow alarm management policies and procedures to be improved across the organization, increase the quality of care delivered, and improve patient safety across all units of the hospital.
Leah Addis is a healthcare writer at ECRI Institute, Plymouth Meeting, Pennsylvania. She can be reached at LAddis@ecri.org.
Kelly Graham is a patient safety analyst at ECRI Institute PSO. She can be reached at KGraham@ecri.org.
Vladimir Cadet is an associate in the Applied Solutions Group at ECRI Institute. He can be reached at VCadet@ecri.org.
Footnote
1 A query of the ECRI Institute PSO database for events occurring during 2013 found more than 800 events with the word “alarm” in the event description and 45 events with “_alarm_” and “_monitor_” in the event description.
References
Cadet, V. (2014). Safe signals: Managing clinical alarm systems for optimal performance. Health Facilities Management, 2, 29-32.
ECRI Institute. (2013a). Best practices in managing health technology. Health Devices, 42(1), 20-8.
ECRI Institute. (2013b). Clinical Alarms. Healthcare Risk Control, 4: Critical Care 5. Retrieved from https://members2.ecri.org/Components/HRC/Pages/CritCare5.aspx
ECRI Institute. (2009). Culture of Safety. Healthcare Risk Control, Suppl A: Risk and Quality Management Strategies 21. Retrieved from https://members2.ecri.org/Components/HRC/Pages/RiskQual21.aspx
ECRI Institute PSO Database. Component of ECRI Institute, Plymouth Meeting, Pennsylvania.
Graham, K.C., Cvach, M. (2010). Monitor alarm fatigue: Standardizing use of physiological monitors and decreasing nuisance alarms. American Journal of Critical Care, 19(1), 28-35. PubMed: http://www.ncbi.nlm.nih.gov/pubmed/20045845
The Joint Commission. (2013). Hospital National Patient Safety Goals. Effective January 1, 2014: Hospital Accreditation Program [online]. Retrieved from http://www.jointcommission.org/assets/1/6/HAP_NPSG_Chapter_2014.pdf
Paine, L.A., Baker, D.R., Rosenstein, B., et al. (2004). The Johns Hopkins Hospital: identifying and addressing risks and safety issues. Joint Commission Journal on Quality and Patient Safety, 30(10), 543-50.
