Satisfied Patients Lower Risk and Improve the Bottom Line
March / April 2008
![]()
Satisfied Patients Lower Risk and Improve the Bottom Line
Most industries have readily accepted that improved customer service will lead to increased customer loyalty, increased revenue, and an enhanced bottom line. However, the healthcare industry has lagged in accepting this concept for several reasons:
- Customers are not loyal in the traditional sense because they usually wish to avoid using the healthcare system, except when necessary, and most executives believe they go to the health facility to which their physician sends them.

- Most customers are insulated from price due to health insurance, and often fail to care about cost, only wanting the best, newest procedures.

- Clinical care is often viewed by physicians as completely separate from traditional customer or administrative service (which is viewed as the admissions, billing, and “hotel” aspects of a medical encounter).

- Clinicians believe great medicine will gain forgiveness for poor service (reinforced by television shows such as House).
But TARP Worldwide’s research and consulting with leading health systems including a large health system in the Midwest, suggests that:
- The customer service aspects of patient interactions with staff are as important as the quality of clinical care provided by physicians in driving patient loyalty.

- Word of mouth is alive and well for both potential patients and referring physicians (who are more loyal to the patient than to other physicians).

- It is possible to quantify the revenue and risk reduction impact of improved experience in a manner that both the chief financial officer and clinicians will accept and appreciate.

- Eliciting and more effectively addressing complaints from patients and their families can lead to double-digit improvements in patient satisfaction scores and reductions in risk costs.
This article outlines the key aspects of this approach and provides case study examples from the Midwestern health system, which achieved an improvement in patient satisfaction of more than 20%, as measured by its ongoing satisfaction survey process, and a significant reduction in risk expense, all in fewer than 18 months.
Patient Behavior Affects Loyalty, Revenue, and Risk
There are many patient and family behaviors that mirror more traditional consumer marketplace environments.
Sources of problems. Most organizations assume that dissatisfaction is primarily caused by the inappropriate actions and attitude of employees. TARP has found otherwise. We have found that most employees come to work wanting to do a good job, but that the environment is not conducive to quality service because of broken policies, procedures, and processes (which cause 50% to 60% of dissatisfaction in most medical care settings). Only about 20% is caused by employees doing something other than what they were told to do. The last 20% to 30% of dissatisfaction is caused by patients who make mistakes, fail to follow directions, or have unrealistic expectations.
Non-complaint behavior. In most markets, TARP finds that 50% of consumers don’t complain about their most serious question or problem. In medical care, the non-complaint rate hovers between 65% and 75%, and some institutions have observed more than 80% non-complaint rates for the patient’s most serious question or problem. For serious medical care and treatment problems (meaning actual or potential adverse medical experiences), usually two-thirds of patients don’t complain.
Reasons patients cited for not complaining (in over 9,000 completed interviews) include 1) the belief that complaining will do no good (what TARP calls “trained hopelessness”); 2) fear of retribution by medical staff, and 3) uncertainty regarding where to complain. This last barrier is further exacerbated if the employees feel that they are not equipped to handle problems. If employees don’t feel comfortable handling complaints, they will avoid encouraging complaints. For instance, when asked what they did if a customer appeared to be dissatisfied, employees in one setting replied, “Keep your head down and don’t make eye contact, then they usually don’t complain.”
Our client found that 70% of patients do not complain and half of the 70% don’t because they feel that it would do no good.1 One of the system’s major action areas at was to train employees regarding how to respond to difficult questions and problems so that they would feel comfortable in eliciting them. Note: an aggressive complaint-solicitation process (described below) can effectively surface these problems before they add to bottom-line damage.
Reluctance to escalate. Even when patients complain in a medical care setting, usually only one-third of them are completely satisfied. Of those who are not completely satisfied, fewer than 5% escalate. In other words, in an average medical care setting, Patient Relations usually only receives about 1 report for every 20 serious (medical care) problems and 1 complaint for every 40 to 50 less serious (service-related) problems.
Ability to discern “robotic empathy.” Patients, like consumers dealing with computer support call centers and overtaxed retail and airline employees, are quick to discern preprogrammed expressions of concern and sympathy (what TARP calls “robotic empathy”). This lack of genuine concern actually becomes an exacerbating factor and makes customers more angry and sensitive to other slights.
Word of mouth. TARP’s general consumer research has always shown that twice as many people hear about a bad experience than a good experience. In medical care, the ratio is two or three to one, depending upon the type of problem. At the Midwestern health system, three acquaintances were told about a good experience, but six were told about a bad experience. Non-complainants still told a median of three friends and neighbors outside their immediate family about their bad experience.
Reticence to take legal action. Several articles in the New England Journal of Medicine and Medical Care indicate that fewer than 3% of patients took legal action, even in adverse medical outcomes where a contributing error was likely (Studdert, et al., 2000; Localio, et al., 1991). A separate study by Studdert and Mello (2006) reviewing 1452 closed claims of five insurance companies went further to find that 40% of the claims reviewed either had no injury or the adverse outcome was not due to an error.
However, 27% of cases where there was no error were still compensated with an average payout of more than $300,000. While the underlying data is not perfect, the findings mirror what TARP has seen in other liability and regulatory environments. In consumer markets, between 1 in 50 and 1 in 300 consumers go to attorneys or regulators when they encounter a serious problem — even if the company was not at fault. In most cases, the cause of escalation is poor handling or inaction up front. The key to reduced risk costs is to intervene in the progression of problems from occurrence, toward claims, lawsuits, and settlements (Figure 1).
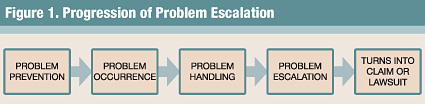
Switching medical care institutions and providers. While clinicians feel that great diagnostic and curative expertise trumps all service problems and behaviors, TARP has found that certain actions and hassles will result in dramatic reductions in willingness to return or recommend. If the patient perceives they have received poor, arrogant, or insensitive care from a clinician, their willingness to recommend or return drops between 30% and 50%. A recent study at Dartmouth University confirmed that almost two-thirds of patients and their families have significant input into decisions about which institution to use for treatment (Wilson, Woloshin, & Schwartz, 2007). Further, in some studies, TARP has found that many patients will complain to the referring physician or primary care physician who, in turn, will stop referring patients. This is in part, we believe, because the primary care physician does not want to receive or have to deal with further complaints about colleagues.
Quantifying the Impact of Less-than-Perfect Service and the Payoff of Service Improvements
It is easiest to identify where the patient experience should and can be enhanced by identifying the problems that lead to serious impact on the bottom line. In addition, organizations should view the stages in problem evolution when damage can be prevented or mitigated.
TARP has identified four major dissatisfiers that can be translated into “market damage.” These can then be mapped back into the patient care process and often can be prevented or mitigated by proactive action:
- Adverse medical outcome, especially when the patient has not been effectively educated on the potential risk of the outcome.

- Inadequate communication, unresponsiveness, or provision of information by a clinician.

- Difficulty gaining access to care (wait times for or during appointments).

- Poor treatment by administrative staff.
Medical care is not totally different from other industries, where bad things happen that are outside the control of the staff (e.g., weather delays and cancellations by airlines). How the institution communicates the potential for these issues to occur and how they are handled can have a dramatic effect on the damage caused to the institution by adverse outcomes.
An additional issue is the situation where there actually has been injury due to a medical error. A direct acknowledgement along with an apology is a good start that conveys goodwill and a desire to improve. This is then supplemented with two other “deliverables”; an action plan on how the institution will mitigate the harm for the patient and an action plan on how the event will be analyzed to prevent similar occurrences. The acknowledgement and apology in conjunction with the two action plans will go a long way toward defusing anger and dissipating the urge to sue. As mentioned earlier, existing research shows that 97% don’t sue, in most cases they are prodded by adverse treatment beyond the original error. One TARP client cut liability costs by 30% via immediate acknowledgement and presentation of an action plan to mitigate the injury.
Quantification of the revenue and risk impact of these issues requires information such as problem prevalence, type, outcome, and revenue value of the average patient, possibly by department. The actual quantification process that TARP uses involves three sets of calculations. First, an estimate is derived of the incremental number of patients who will return to the institution because of reduced problem experience and how the problems are handled. Second, the incremental referrals due to positive word of mouth and reduced negative word of mouth are calculated. Finally, the reduction of risk expense due to better up-front handling of problems is estimated. In all three calculations, input and agreement from finance are essential (Goodman, O’Brien, & Segal, 2000). Negotiate conservative estimates of any underlying assumptions with the CFO so that when the business case for investment in service and quality is presented, the CFO will accept the validity of the estimate.
Once these factors have been quantified, the current situation can be mapped out, and the revenue “left on the table” and extra cost being incurred can be calculated. Then opportunities can be quantified in terms of problems prevented, additional problems identified and handled to satisfaction early, and potential risk situations prevented by better problem handling.
Finally, scenarios with improved problem rates, complaint rates, and resolution rates can be developed to calculate the “after” scenario using the new parameters. These can include higher positive resolutions and word of mouth and lower amounts of negative word of mouth. The difference between the “before and after” scenarios will highlight the bottom-line opportunity in a manner that is relatively transparent to the CFO — he or she can see exactly how the numbers were developed.
The results of the above analysis can be used to create the economic imperative to improve service. The best way to create momentum is quantify. For example: “For each month of inaction regarding these issues, the organization is leaving $2 million on the table and incurring $400,000 in unnecessary risk and complaint handling cost.” Knowing the cost of inaction inspires action.
Strategies for Enhancing Service
TARP recommends four strategies for enhancing the bottom line via improved loyalty, word-of-mouth marketing, and risk reduction.
1. Enhance the ability of front-line personnel to respond effectively to the top four to six problems. Identify clear explanations regarding why negative events can occur and suggest actions that staff can take to mitigate the patient’s dissatisfaction. Think of airline flight cancellations that were handled well and those that were handled badly: The key difference is how the staff interacted and communicated with customers. The same effective responses can be designed for treatment delays and most adverse outcomes.
A key part of the formula is an initial empathetic, apologetic response. This apology can be made without accepting blame on the part of the organization if you don’t yet have all the details, e.g., “I’m sorry you’ve been inconvenienced.” But responsibility should be accepted if you discover someone in the organization dropped the ball, e.g., “I’m sorry someone didn’t return your call.” This factor is supported by an article in Surgery, which reported that the “Surgeons’ tone of voice in routine visits is associated with malpractice claims history” (Ambady, et al., 2002). A second component is the ability to say “no” to the customer when necessary — employees must be able to provide a clear, believable explanation of the reason they are not able to comply with the customer’s request.
It is imperative that this explanation be plausible from the customer’s perspective and not be merely an excuse. To use another example from the travel industry: Contrast an announcement that a flight is delayed or cancelled due to “mechanical difficulties,” which could cause passengers to question the airline’s competence at a number of levels, with an approach that apologizes for the delay and explains the need to repair a defective hydraulic system because passenger safety is paramount. Passengers may still be unhappy about the delay but the explanation is likely to move them from dissatisfied to mollified or somewhat satisfied.
At our client in the Midwest, all staff members, including physicians, were trained in creating positive first impressions, effective communication, teamwork, and service recovery for addressing the most prevalent problems. To ensure acceptance by staff, more than a dozen physicians were recruited as trainers by the CEO, who is also a physician.
2. Work to prevent the top four to six problems by fixing processes and by proactive patient education. Organizations can prevent problems by improving processes, especially if the economic imperative for the solution can be established. In addition, actively educate patients regarding possible adverse outcomes (i.e. tell them more than “read and sign the release”). TARP has found that when the two or three most likely negative outcomes are explained, and the customer actively acknowledges hearing them, patients are much less upset if they do occur, because they have been forewarned. In general, we find that even though patients may not be completely satisfied, keeping them informed reduces anger and punitive action. At the Midwestern health system, a key part of prevention was identifying problems by logging them on the Patient Services Report. Once logged, it was possible to both track and analyze causes and move from firefighting into a preventive mode through proactive communication. It was critical that staff know that the analysis was to identify processes rather than people to blame.
3. After implementing effective response processes (Step 1), aggressively elicit complaints. Raise the visibility of the organization’s complaint-handling process. Place messages stating that “We can only solve problems we know about!” in front of patients exactly where they may encounter the problems. For example, in one ob-gyn department, TARP designed signs that said, “Please tell the front desk if you are upset and or call us at Patient Relations!” The signs were located next to an in-house phone and indicated the extension for Patient Relations. Complaints increased, but overall satisfaction scores also increased significantly.
At the Midwestern health system, the visibility and emphasis of the patient bill of rights was significantly enhanced so that patients were consciously educated that the organization wanted to hear about problems and where to complain. This document was not treated just as a notification to be signed and glossed over but was used to reinforce with the patients that the institution could only address problems brought to its attention and that it really did want to know.
TARP has found the same approach can significantly reduce regulatory complaints. If patients know about an appeals or ombudsman mechanism that is internal to the institution (especially if it is confidential), TARP has found that patients will go there first rather than going to attorneys or regulators. In several regulated environments, TARP raised the visibility of internal customer advocates and saw escalations to regulators or attorneys decline by up to 50%.
4. Provide a highly visible Patient Relations function. This is related to the previous recommendation. The Patient Relations function must have two key components. First, Patient Relations must be able to resolve issues in a rapid, non-bureaucratic fashion, and it must be fully empowered to resolve issues prior to patients going to attorneys or regulators.
Second, Patient Relations must also be able to gather data on the entire sequence of events, including exacerbating factors that led to a situation. Except for the most serious adverse medical events, almost all escalated complaints are escalated for a reason other than the original problem, whether it was an uncaring response, no response, or another form of disrespect. This analysis of root and contributing causes is critical to Patient Relations being able to actively improve the process and deliver an improved bottom line.
Our client created a customer service department in 2006. Any issue that has risk potential is analyzed to determine what service or communication process led to it — processes are blamed, not people. Then actions are taken to rectify the problem with the patient, and improve the process for those prevalent issues that caused the most damage.
Summary
Our client in the Midwest has experienced a substantial increase in patient satisfaction scores. The system has increased its rank to above the 90th percentile in overall satisfaction at each of its four regional emergency departments, as measured by the ongoing patient survey process. After analyzing data from patient complaints, patient satisfaction scores, and service recovery expenditures, the system determined that action was needed in its ambulatory surgery area to respond to the number of complaints regarding delay and its mediocre patient satisfaction scores.
Staff and physicians responded by increasing communication to waiting patients and families, increasing the use of service recovery tools, and following-up with patients post-surgery if they had experienced a delay. This quick action by staff and physicians was met with almost immediate results. Within 3 months, patient satisfaction scores rose from the 53rd percentile in the nation to the 89th percentile in overall ambulatory surgery satisfaction. Also, risk exposure has been significantly reduced, by a double-digit percentage.
The number of complaints is up, but management believes that service is actually better, and patients are more comfortable reporting problems so the problems may be addressed. Complaints are viewed as positive opportunities to address issues: “bad” is now defined as a dissatisfied patient.
In summary, in many medical care institutions, Patient Relations is viewed as a necessary but costly expense. However, every dollar spent on the Patient Relations function is probably returning from 200% to 500% in terms of reduced revenue losses and risk expenditures, and enhanced positive word of mouth. However, to be able to quantify the impact in a manner the CFO will accept, Patient Relations and Quality need to assess the full sequence of events when problems and adverse events occur in the course of medical-care delivery, evaluate how they are addressed, and close gaps in service quality. Our client’s focus on addressing problems at point-of-service, both by front-line staff and physicians, and by dedicated customer service personnel, has led to an increase in knowledge of patient and family expectations, and to a lessening of the impact of any potential risk management issue. This strategy, of course, benefits both the patient and the healthcare organization.
1 Survey of over 20,000 patients, over 3,900 returns, 2004.
John Goodman is vice chairman of TARP Worldwide. In 1972, Goodman was a founding member of TARP, a research and consulting organization that specializes in customer service and quality improvement. He has managed more than 800 separate customer service studies, including TARP’s White House-sponsored evaluation of complaint handling practices in government and business; studies quantifying word-of-mouth, and the bottom-line impact of consumer education. He has taught courses on quality measurement and improvement for Wharton Business School Executive Education and the American Society for Quality. Goodman graduated from Carnegie Mellon University with a BS in chemical engineering. He received an MBA from Harvard Graduate School of Business Administration. He may be contacted at jgoodman@tarp.com.
Dianne Wardis senior account manager at TARP Worldwide. She has extensive experience managing customer satisfaction/loyalty research projects, with special expertise in conducting qualitative assessments of clients’ customer/member service systems, and interpreting research findings to drive service quality improvements. Prior to joining TARP in 1993, Ward was with the National Council of Better Business Bureaus (CBBB) as director of public affairs and national manager of mediation services. Ward holds BS and MA degrees in business and consumer studies from Michigan State University, both magna cum laude.
References
Ambady, N., LaPlante, D., Nguyen, T., Rosenthal, R., Chaumeton, N., & Levinson, W. (2002, July). Surgeons’ tone of voice; A clue to malpractice history. Surgery, 132, 5 — 9.
Goodman, J., O’Brien, P., Segal, E. (2000, March). Turning CFOs into quality champions. Quality Progress.
Localio, A. R., Lawthers, A. G., Brennan, T. A., Laird, N. M., Herbert, L. E., Peterson, L. M., Newhouse, J. P., Weiler, P. C., & . Relation between malpractice claims and adverse events due to negligence. Results of the Harvard medical Practice Study III. New England Journal of Medicine, 325, 245 — 251.
Studdert, D. M., Mello, M. M., Gawande, A. A., Gandhi, T. K., Kachalia, A., Yoon, C., Puopolo, A. L., Brennan, T. A.. (2006, May 11). Claims, error, compensation payments in medical malpractice litigation. New England Journal of Medicine, 354, 2024-2033.
Studdert, D. M., Thomas, E. J., Burstin, H. R., Zbar, B. I. W., Orav, E. J., Brennan, T. A. (2000, March). Negligent care and malpractice claiming behavior in Utah and Colorado. Medical Care, 38(3), 250-260.
Wilson, C. T., Woloshin, S., & Schwartz, L. (2007, March). Choosing where to have major surgery: Who makes the decision? Archives of Surgery, 142, 242-246.
