Perioperative Pressure Injuries: Protocols and Evidence-Based Programs for Reducing Risk
A study of 21,377 surgical patients screened with the Scott Triggers Tool found that more than 7,000 patients had two or more triggers and were considered to be at high risk for pressure injury (Martinez et al., 2014). For these patients, an OR skin bundle was implemented that included skin assessment on admission, transfer, and discharge; standardization of high-specification OR table pads; interprofessional education; careful positioning; redistribution and offloading of pressure; protective dressings; frequent assessments; turns scheduled every two hours using wedges; and real-time reporting of pressure injuries. Results showed the rate of HAPI decreased from 3.37% to 0.89% (p=0.004), with the reduction sustained over a 14-month period. The facility also lowered costs by nearly $1.4 million over a one-year period (Martinez et al., 2014).
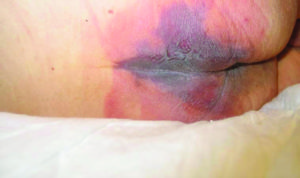
High-specification OR table pads
To more effectively redistribute pressure on the bony prominences of the body, the surface of the OR table should allow for immersion of the body into the material. Standard OR table pads are comprised of a 2-inch elastic foam covered with black, conductive, laminated vinyl fabric. While this type of pad is great for stability, several studies have demonstrated that it contributes to pressure injury development during surgery (Aronovitch, Wilber, Slezak, Martin, & Utter, 1999; Feuchtinger, Bie, Dassen, & Halfens, 2006; NPUAP, 2014; Nixon, McElvenny, Mason, Brown, & Bond, 1999; Russell & Lichtenstein, 2000; Schoonhoven, Defloor, & Grypdonck, 2002; Scott, 2013).
High-specification foam mattresses, on the other hand, have been shown to reduce the development of pressure injury (McInnes et al., 2015; Scott, 2015). Soft, multi-layer cushions allow patients to sink into the underlay, with the cushion molding around the patient’s body to increase surface contact by up to 60%. This helps distribute pressure across a greater area. Bi-elastic covers also reduce creases and shear forces on the skin. While installing new OR table pads is an added expense, intraoperative prevention may be more cost-effective than the current practice (Pham et al., 2011). At the VA Medical Center in Memphis, replacement of all OR table pads resulted in a reduction in the cost of extra foam positioning devices by $250,000 over two years.
Implementing a Perioperative Pressure Injury Prevention Program
Implementing a Perioperative Pressure Injury Prevention Program (PPIPP)—previously known as a Perioperative Pressure Ulcer Prevention Program or PPUPP—is another strategic way to reduce HAPI in the acute care setting. After a PPIPP was instituted at the VA Medical Center in Memphis, the incidence of HAPI fell 60% over a four-year period, with a cost avoidance of $3.1 million (Scott & Hector, 2001). Recognized by the American Academy of Nursing (2016) as an innovative approach to improving healthcare through nursing leadership, a PPIPP has been used successfully in the Veterans Integrated Service Network, where it reduced costs by $2.4 million in a single fiscal year.
PPIPP includes a 10-step strategy to strengthen HAPI prevention efforts:
- Quality improvement. Using the DMAIC improvement model (define, measure, analyze, improve, control), bring together an interprofessional team of stakeholders to develop a strategy that addresses barriers to providing optimal patient safety. Determine the facility’s incidence of HAPI by tracking occurrences of pressure injuries and conducting patient safety investigations, including root cause analysis.
- Assessment. Perform a gap analysis and assess the environment. Use the SWOT analysis format (strengths, weaknesses, opportunities, and threats) to set priorities and create an action plan for improvement.
- Staff education and awareness. Develop educational programs for all perioperative staff. Improve awareness by posting the incidence and prevalence of HAPI. Include PPIPP in orientation, staff meetings, and in-service time.
- Evidence-based practice. Incorporate evidence-based national guidelines such as those from the NPUAP (2014) and the Wound, Ostomy and Continence Nurses Society (www.wocn.org) into clinical practice routines.
- Risk assessment. Numerous risk factors have been linked to pressure injury development in surgery. Decide which tool or tools best fit your setting. The Braden Scale should be used in conjunction with other “surgical-specific” tools such as the Scott Triggers Tool or Munro Scale for identification of at-risk individuals (Putnam, 2016). Consider additional factors such as surgical case type, position, trauma, and reoperations.
- Perioperative nursing care plan. Use an OR skin bundle tailored to your surgical setting. Incorporate a system redesign to standardize care for all patients. Develop or refine structured, standardized handoff communication to include surgical position, time on the table, and skin assessment in your SBAR (situation, background, assessment, recommendation) tools and verbal reports. Documentation should be clear and concise and include nursing interventions and assessments. Complete documentation may also help protect against litigation.
- Positioning competencies. Integrate guidelines for perioperative positioning from the Association of periOperative Registered Nurses (AORN) (2015) into clinical practice.
- Universal pressure precautions. Incorporate pressure redistribution and relief devices into all perioperative care. Start by standardizing high-specification support surfaces in all functioning ORs and on beds/stretchers prior to and after surgery. Use of a high-specification support surface on the operating table for at-risk individuals is recommended (NPUAP, 2014). Devices used for positioning and padding should be consistent with principles of pressure redistribution, as this is the cornerstone for success (Black, Fawcett, & Scott, 2014; Scott, 2015).
- Product specification and selection. There is insufficient evidence to conclude which surfaces and devices are most effective for prevention; however, review of available clinical research and outcome studies on all positioning devices is recommended (Scott, 2015). Prior to purchasing a product, consult with a team to develop specific criteria for product selection consistent with your environment: safety features, fire standards, biomedical requirements, infection prevention, decontamination, resuscitation, radiolucency, weight limits, and efficacy. Is the product compatible with tables and positioning requirements? Consider the initial and replacement costs, disposable vs. reusable products, applicable warranty, and manufacturer reputation.
- Specialty nurse collaboration. Improve handoff communication and collaboration between the interprofessional team of perioperative staff: post-anesthesia; wound, ostomy, and continence nurses; and nursing.
