Making It Easy for Nurses to Reduce the Risk of CLABSI
Making It Easy for Nurses to Reduce the Risk of CLABSI
By Wendy Kaler, CLS, MPH, CIC
Increased compliance with the 2002 Centers for Disease Control and Prevention (CDC) Guidelines for Prevention of Intravascular Catheter-Related Infections (O’Grady, Alexander & Dellinger, et al. 2002) resulted in a significant decrease in early stage (less than 4 days) central-line associated bloodstream infections (CLABSI) (Furuya, et al.; 2011; Shulman et al., 2011). The patient safety challenge that remains is to reduce the number of preventable CLABSI that occur beyond 4 days as a result of non-compliance with maintenance bundles. Although contamination can arise from infused solutions and within IV tubing, there are two main paths of entry for microorganisms that may contribute to preventable infections during the indwelling period: extraluminal (at the point where the line enters the skin) and intraluminal (from catheter hubs and needleless connectors).
To address extraluminal infection, chlorhexidine products may be delivered to the skin at the insertion site to provide a standardized approach to reduce risk. This practice has become universal by standardizing the products that are purchased so that no other option is available in dressing-change kits for insertion and vascular access devices. However, due to the number of times hubs are accessed during the indwelling period, this intraluminal portal of entry for bacteria remains at high risk for microbial ingress.
During 22 years as a practicing infection preventionist, I’ve had ample time to consider the challenges of central-line associated blood stream infections (CLABSIs). Although I have seen vast improvements on many fronts, consistent and effective disinfection of needleless valves is one area of practice that has received little attention. It became the focus of my research in 2007 and the ongoing focus of my current institution, a large community hospital in the San Francisco Bay area. I conducted a study (Kaler & Chinn, 2007) that proved 15 seconds of exposure to 70% alcohol applied with friction was effective to disinfect an access port contaminated with high levels of bacteria. This amount of bacterial burden is consistent with what likely would be found on the surface of a port in contact with a patient’s skin.
When approaching needleless access ports, nurses must always assume they are contaminated. For a time-challenged nurse, a full 15 seconds of scrubbing every time a port is accessed is demanding. When The Joint Commission updated its National Patient Safety Goals to include, “Use a standardized protocol to disinfect catheter hubs and injection ports before accessing the ports”(NPSG#07.04.01 Element 12), we needed to implement a compliance monitoring system. Because nursing staff will modify their practices when they know they are being observed, catheter hub disinfection is nearly impossible to monitor accurately. When no one is looking, does anyone clean those ports? And how often does a nurse simply forget to do it? Anonymous surveys, vendor observations (during smart infusion pump conversions), and questions posted on email discussion groups made it clear that no standard practice was in place.
CLABSIs are irrefutably life threatening—12 to 25% of these infections end in death (CDC, 2011)—and they are costly to treat, averaging more than $45,000 per case (Zimlichman et al., 2013). Recognizing the preventability of CLABSI, the Centers for Medicare and Medicaid Services (CMS) holds back payment to healthcare organizations that report higher than predicated rates of CLABSI (risk-adjusted for their patient population). Currently, CMS denies reimbursement under its value-based purchasing guidelines for CLABSI cases that occur in the ICU, but the proposed 2020 CLABSI goals (CMS, 2014) will expand this rule to include all patients on all wards. This expanded focus will result in a loss of hundreds of thousands of dollars to hospitals, impacting the bottom line of those that have not yet implemented successful strategies for CLABSI reduction.
A Novel Approach — Creating a New Normal
 |
|
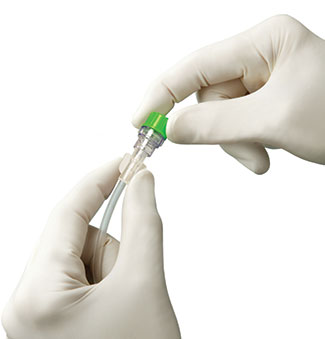
| Figure 1. A single-use disinfecting port protector securely luer-locks onto a needleless connector. |
In 2009, I was informed that alcohol port protectors were available for purchase. I had been teaching the 15-second hub scrub as a standard in my hospital, with varying degrees of acceptance and compliance based on nursing staff interviews. I was pleased to find a product that could hardwire a disinfection practice, which I was, at that time, unable to validate with scrubbing. With single-use disinfecting port protectors, when a line is placed, a nurse needs only to peel the foil seal from the cap impregnated with 70% isopropyl alcohol and twist the luer-lock device onto the needleless connector (Figure 1). The port protector will disinfect and protect the valve’s surface until it is removed for the next access. At that time, the cap is twisted off and the line is accessed with no need for scrubbing. When the access is complete, the nurse places a new port protector on the valve. In this way, port protectors change the paradigm from valves being always contaminated to being always disinfected and ready for access.
I brought the products (three different manufacturers) into my ICU for a trial period. At the end of the trial period, I asked my ICU nurses, “Knowing your current compliance with alcohol scrubbing of IV ports for 15 seconds, if you were the patient, would you feel safer if there were alcohol port protectors covering your ports?” Their response was a unanimous “Yes!”
This represented a paradigm shift; nurses could assume the ports they approached were clean. This was a shift that authors of the CDC 2011 Guidelines had not yet considered when they published the section on port disinfection; the technology was too new to evaluate. The recommendation in the current guideline assumes that the ports are uncovered and contaminated, thus the concept of passive disinfection (versus manual scrubbing) was not evaluated. Nurses who had been compliant with the 15-second hub disinfection were the most vocally supportive of the alcohol port-protector implementation; they appreciated that alcohol port protectors saved them significant time in properly disinfecting ports prior to accessing them.
We started by using alcohol port protectors only with central-line ports because we wanted to focus on the lines with the most significant risk for infection. In order to ensure that the product had been fully implemented throughout the facility, our IV team incorporated a visual confirmation of alcohol port protectors into their daily bedside audits of all central lines. Even though our nurses verbalized support, and we implemented bedside coaching by the IV team for bedside nurses, the highest compliance we were able to achieve with the caps on central lines was 85%. Because we know just one lapse can lead to CLABSI risk, our goal is 100% compliance.
We found that many nurses wanted to use alcohol port protectors on all ports including those on peripheral lines (PIVs), and we learned that nurses were confused when patients had both central and peripheral lines. Why should they cover one but not the other? Many ports could be the source of infections, but when reporting blood stream infections (BSI) into the National Healthcare Safety Network (for CMS reporting), we have to attribute any BSI experienced by a central-line patient to the central line, regardless of which access site might be the origin of the infection. In order to achieve higher compliance on the highest risk central-line ports and reduce the risk of all catheter-related blood-stream infections, which accounted for a standard peripheral IV infection rate of 0.5/1000 catheter days, we chose to use the caps on all IV access ports. No longer did each individual nurse have to decide which port to cover. The rule was universal; every port would have an alcohol port protector. This shift to one standard protocol drove change and created a new normal; as a result, we quickly reached 98 to 100% compliance.
Sustaining the New Normal
 |
|
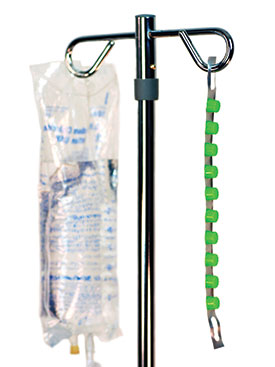
| Figure 2. When hung on the IV pole bedside, disinfection caps are convenient for nurses to access. |
Over the years, I have learned the importance of assigning an individual or “point person” for any new product implementation. In our hospitals, we find that all product or procedure roll-outs must be considered to be temporary unless there is intensive shepherding by designated individuals who maintain vigilance until the change is hardwired. In most cases, the champion of CLABSI prevention is an infection preventionist (IP). To reduce publicly-reported infection rates in their healthcare systems, performance improvement has become a key role for IPs. Periodic spot checks must be made (every three months) to confirm that the product is still available to the end user, as products get moved or removed entirely from supply carts on units due to space limitations and competing priorities. Product needs to be in a convenient place where nurses do not have to hunt for it. This can be accomplished with a variety of approaches including placing the product on IV carts next to the tubing sets or attached to an IV pole at the bedside (Figure 2).
Audits are a reality for any performance improvement program; otherwise, we live in a fantasy world where we believe our programs are implemented, blind to real breakdowns in practice. To drive change, auditing has been adopted by many regulators, including the state of California, which requires documentation of central-line insertion practices (CLIP) in all critical care units. Regular checks are important for sustaining results. Alcohol port protectors are readily visible to an auditor, providing a clear indication that hubs have been disinfected.
In addition, engaging the end user is imperative. Bedside nurses have limited time for competing priorities, so champions must appeal to them by personalizing the value of implementing new products. Using meaningful phrases that appeal to the individual’s sense of personal safety is important, such as, “If your best friend were lying in that bed, would you want to see alcohol port protectors on their IV ports?” Ultimately what we must do to make the environment safer for our patients is to provide support, including products that make it easier for staff to keep our patients safe.
Champions must be helpful, supportive “cheerleaders,” not enforcers. In Slow Ideas, Atul Gawande (2013) explains that the way standards change is not by providing incentives or punishment but by “people talking to people.” When people are made aware their actions put patients at risk and are then provided an appealing and timesaving way to reduce that risk, they are more apt to become adopters.
 |
|
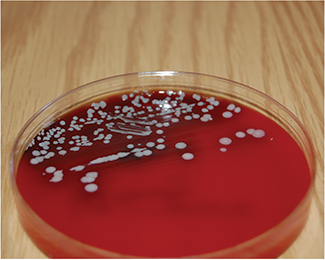
| Figure 3. Bacteria cultured from unprotected IV port. |
One strategy I often use in support of alcohol port protectors is to show nursing staff a photo of a petri dish culture of the surface of a needleless cap that had been on the patient’s skin for a few days (Figure 3). The visual demonstration of the bacterial colonies illustrates the risk they could not see with their own eyes until that moment. During this conversation, I have seen nurses become engaged and awakened to the reality of the risk of infection transmission attributable to their own practices. Once they are aware, I find that they become willing participants and freely provide creative feedback on how to improve compliance. A champion who is accessible to them—someone who will listen and act on their feedback—is often lacking. In order to ensure full penetration, champions who audit and assist with implementation must be on the nursing units periodically for months, long after the product is brought into a facility. Easy-to-visualize alcohol port protectors can be audited by unskilled workers as well as members of the C-suite during leadership rounding. It is imperative that a hospital not falsely believe that they have full implementation of an alcohol port protector when they do not; otherwise, they are likely to misclassify the root cause of a line-related sepsis.
The Joint Commission requires that patients with central lines be provided information regarding the strategies being used to prevent line infections (The Joint Commission, NPSG 07.04.01, 2014). Patients are educated regarding the role of the alcohol protectors and are able to take an active role in reminding staff to keep their ports properly covered. We hope that this visible patient safety program adds to patient satisfaction and confidence in our dedication to their safety.
Conclusion
Lower CLABSI rates are achievable with well-supported programs that include staff awareness of infection risks combined with full implementation of alcohol port protectors. The result is a patient safety practice that is easy for nurses to follow and easy for everyone to see in action.
Wendy Kaler has been a practicing infection preventionist for 22 years. She has served on expert panels for CLABSI prevention, CAUTI prevention, and surface disinfection. She has presented her strategies for reducing CLABSI to numerous professional organizations across the United States. She is currently the director of infection prevention at Saint Francis Memorial Hospital in San Francisco, California. Kaler may be contacted at wdkaler@gmail.com.
Kaler, W. (2014). Making it easy for nurses to reduce the risk of CLABSI. Patient Safety & Quality Healthcare, 11(6), 46–49.
References
Btaiche, I. F., Kovacevich, D. S., Khalidi, N., & Papke, L. F. (2011, May). The effects of needleless connectors on catheter-related bloodstream infections. American Journal of Infection Control, 39(4), 277-283.
Centers for Disease Control and Prevention (2011). Vital signs: Central line-associated bloodstream infections—United States, 2001, 2008, and 2009. Morbidity and Mortality Weekly Report, 60(8), 243-248. Retrieved from http://cdc.gov/mmwr
Centers for Medicare and Medicaid Services. National action plan to prevent health care-associated infections: Road map to elimination. Retrieved from http://www.health.gov/hai/pdfs/HAI-Targets.pdf
Crnich, C. J., & Maki D. G. (2014, June) Chapter 34 Intravascular Device Infection. APIC Text of Infection Control and Epidemiology, 4th Edition. Retrieved from http://text.apic.org/item-35/chapter-34-intravascular-device-infection
Eggimann, P., et al. (2000, May 27). Impact of a prevention strategy targeted at vascular-access care on incidence of infections acquired in intensive care. Lancet, 355(9218), 1864–1868.
Furuya, E. Y., et al. (2011, January 18). Central-line bundle implementation in US intensive care units and impact on bloodstream infections. PLoS One, 6(1), e15452. Retrieved from http://www.plosone.org/article/info%3Adoi%2F10.1371%2Fjournal.pone.0015452
Gawande, A. (2013, July 29). Slow ideas. The New Yorker. Retrieved from http://www.newyorker.com/magazine/2013/07/29/slow-ideas
The Joint Commission, 2014 National Patient Safety Goals. NPSG#07.04.01 Element 12, p 10. Retrieved from http://www.jointcommission.org/assets/1/6/HAP_NPSG_Chapter_2014.pdf
Kaler, W. & Chinn, R. (2007). Successful Disinfection of needleless mechanical valve access ports: A matter of time and friction. Journal of Vascular Access, 12(3), 140-142.
Mermel, L. A. (2000). Correction: catheter-related bloodstream infections. Annals of Internal Medicine, 133, 395
O’Grady, N. P., et al. (2002). Guidelines for the prevention of intravascular catheter-related infections. Morbidity and Mortality Weekly Report. 51(RR-10), 1-26.
Schulman, J., et al. (2011, March). New York State Regional Perinatal Care Centers. Statewide NICU central-line-associated bloodstream infection rates decline after bundles and checklists. Pediatrics, 127(3), 436–444.
Zimlichman, E., et al. (2013). Healthcare-associated infections a meta-analysis of costs and financial impact on the US healthcare system. JAMA Internal Medicine, 173(22), 2039-2046.
