Insight in Preparedness for Healthcare Facilities
By James D. Ferris, PE, and Aaron Johnson, PE, LEED AP BD+C
The advent of the COVID-19 pandemic in 2020 brought the need for emergency preparedness in hospitals and medical facilities to the forefront of nearly every discussion in the industry. Today, with the delta variant fueling another surge in cases across the United States, the challenges continue. With different rules and regulations in every state, the protocols for controlling the virus vary depending on the hospital system.
Because utility infrastructure impacts every area of hospital operations, from the day a new hospital is opened and for many decades to come, it is important to understand key decision drivers when developing emergency preparedness plans.
Here, we will analyze several of the key drivers of hospital/medical facility planning and design required to meet future needs—including the need for energy efficiency, an understanding of available redundancy, and a comparison of first costs versus life cycle costs.
Energy efficiency
Hospitals and medical facilities face a number of challenges in achieving their desired energy efficiency. Having flexible systems capable of accommodating normal operations and expending the energy required for emergency conditions, such as a pandemic mode, is key.
From a wellness standpoint, the goal is to have the flexibility to conserve energy year-round in normal operational circumstances, but also have the ability to easily pivot to a system that provides improved air quality based on the needs of the current environment and the level of protection necessary for staff.
For example, the air quality and exhaust needs for COVID-19 are different from those for other airborne illnesses. There are greater precautions needed for staff safety and comfort—whether that involves introducing or increasing the fresh air intake from outside, or augmenting existing ventilation systems.
According to calculations from the U.S. Environmental Protection Agency (EPA)’s Energy Star program, hospitals consume more than 315 gallons of water per bed every day and the average U.S. hospital consumes 103,600 Btu of natural gas per square foot annually. In addition, lighting, water heating, and space heating account for more than 65% of the energy consumption.
The EPA estimates that every $1 a nonprofit healthcare organization saves on energy equals generating $20 in new revenues for hospitals (or $10 for medical offices). Therefore, investing and focusing on energy-efficient utility infrastructure systems can help healthcare organizations fund emergency preparedness programs from savings generated through improved energy performance.
A building that functions more efficiently has greater run times and higher performance in the event of a power outage. A comparison between energy use in an efficient versus a less efficient building often will show that the efficient facility can function 40%–50% longer on the same gallon of fuel used by an emergency generator. Energy savings have an immediate and direct impact on the reduction of operating costs.
One of the simplest ways for owners to optimize spending is to review their energy utility bills. Often, such bills are expedited—sent to accounting and paid. However, even a cursory analysis from an expert often can unearth potential gaps in efficiency, such as a valve left open or a water leak, simply by comparing the way the utility data is trending.
Understanding available redundancy
Hospitals are required by code and CMS regulation to ensure critical power supply and infrastructure system functionality. As a result, healthcare leaders aim to build utility infrastructure redundancy into projects—whether new construction, additions, or renovations.
If not engineered appropriately, addition or renovation projects can chip away at original redundancy levels and negatively impact operations. Maintaining redundancy consistent with the capacity for available growth is the best approach to optimize potential. For example, having a higher equipment load than necessary could create a risk of overload, but in some ways, wasting available energy is almost worse.
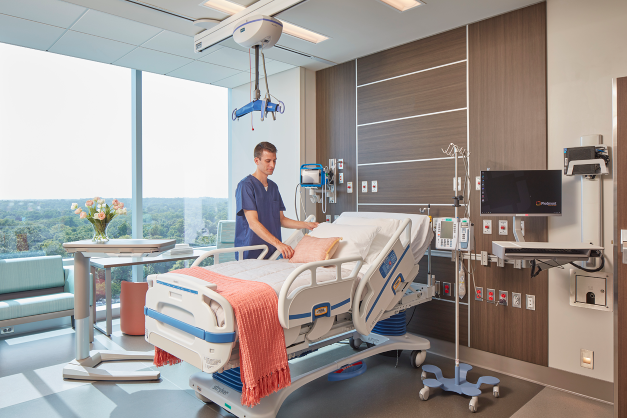
In the case of a 50% load, some unused energy could be applied to functions that do not have a high energy demand, such as TVs in patient rooms. These are not critical to operations, but they help keep patients calm and occupied during an emergency event, relieving the burden of care from staff and allowing them to address the situation with fewer distractions.
Whether it is redundant sources of power or redundant equipment, healthcare leaders must understand the available redundancy as well as the associated risk.
One of the most often misunderstood factors is the risk (i.e., a facility’s level of risk due to not having full redundancy in one of the major components). For example, a facility may have a boiler system that operates with natural gas alone. The system has six boilers when only five are needed, making one redundant.
In this case, the risk is the facility does not have a redundant fuel source for the boiler. This, in turn, begs the question, “What if something happens to the natural gas main and shuts down hospital operations?” Essentially, this facility has redundancy as far as having the ability to take a boiler down for servicing, but it does not have redundancy in regard to the overall fuel source—which, if lost, would force crucial hospital operations to shut down.

Facility leadership aims to know, appreciate, and understand the need for available, multilevel redundancy in planning for preparedness. Hospitals can consider conducting a campuswide utility master plan assessment to accurately calculate available redundancies and ensure sufficient backup capacity to maintain operations in an emergency situation.
Part of preparedness planning is carefully considering interrelated possibilities: “What would happen if something went wrong with each system?” In one example, a hospital had two separate emergency systems, but with such interrelated redundancy, those systems nearly canceled each other out. Operating rooms were on system A and prep/recovery rooms were on system B, and when the hospital took a critical look at how it would operate in an emergency, it realized a failure in either system would render it incapable of performing surgery.
Another facility color-coded a patient floor to show how five generators were backing up different parts of the treatment area, with connections interspersed throughout the floor. The interrelated analysis showed that it would be difficult to manage operational risk because an outage in any one of the generators would affect the entire floor.
First costs vs. life cycle costs
Many hospital leaders understandably focus on construction costs. However, project teams need to enable them to also consider what will be spent over the estimated 50-year (or longer) life of the building.
All too often, project teams do not provide decision-makers with such data. As a result, many project decisions are based on first costs rather than life cycle costs because decision-makers have not been provided information to factor the intrinsic value of “future proofing” spaces.
The reverse should be standard practice. For example, in the planning of greenfield hospitals, leaders could consider installing larger medical gas pipes that can accommodate four times as much as typically required. Why? This allows the hospitals to easily upgrade med/surg floors to isolation rooms, or accommodate for specific needs, at a fraction of the overall construction cost. The COVID-19 pandemic has shown how a large concentration of a specific type of illness can affect medical gas needs—in this case, oxygen. During COVID-19 surges in patient population, facilities have seen oxygen usage 10–15 times higher than normal.
Prioritizing expenditures based on short- and long-term ROI is an important part of the decision-making process. Glass windows are a good example as they don’t get replaced very often, especially in hospitals. Therefore, investing in premium-quality windows can pay dividends for up to 50 years, whereas a chiller or an air handling unit is only going to last 15–20 years at best.
Aspects such as the building envelope and structure, as well as site orientation, are long-term strategies and investments that make a significant difference in costs over the life cycle of the building. Just as there is an optimal traffic flow into and out of the site, there also is an optimal flow of energy in terms of exposure to the elements. Neither can be ignored. Optimizing these decisions will be passively advantageous, regardless of what systems are used inside the building.
The pandemic has heightened the awareness and importance of such flexibility, which is leading decision-makers to take a life cycle analysis approach to resiliency decisions.
Many leaders now are enduring costs due to the pandemic as decision-makers strategize how to retrofit their projects to optimize safety. For example, one of the shifts is upgrading HVAC systems with controllable flexibility within rooms and throughout entire floors.
Some items that had traditionally been on the “wish list” have come to the forefront as necessities in the COVID-19 era. They include sophisticated air handling systems that change the airflow on demand to such an extent that an entire floor can become a negative suite.
Utility infrastructure is crucial to ongoing hospital operations, making these issues—energy efficiency, an understanding of available redundancy, and a comparison of first costs versus life cycle costs—critical in the development of an emergency preparedness plan.
James D. Ferris, PE, is chief operating officer with TLC Engineering Solutions®. He can be reached at james.ferris@tlc-eng.com. Aaron L. Johnson, PE, LEED AP BD+C, is managing principal with TLC Engineering Solutions. He can be reached at aaron.johnson@tlc-eng.com.
