Industry Focus—Infection Control: Examine Your Dialysis Space to Ensure Room to Separate Infectious Patients
This Industry Focus article on infection control is sponsored by Tru-D Smart UVC.
By A.J. Plunkett
Hemodialysis is one of four areas The Joint Commission (TJC) says it’s increasing focus on during surveys. With this in mind, ensure that your hospital’s hemodialysis patients remain in clear view of staff while undergoing the procedure. In addition, make sure there’s enough space to separate patients with respiratory illnesses, fevers, fecal incontinence, or other infectious conditions.
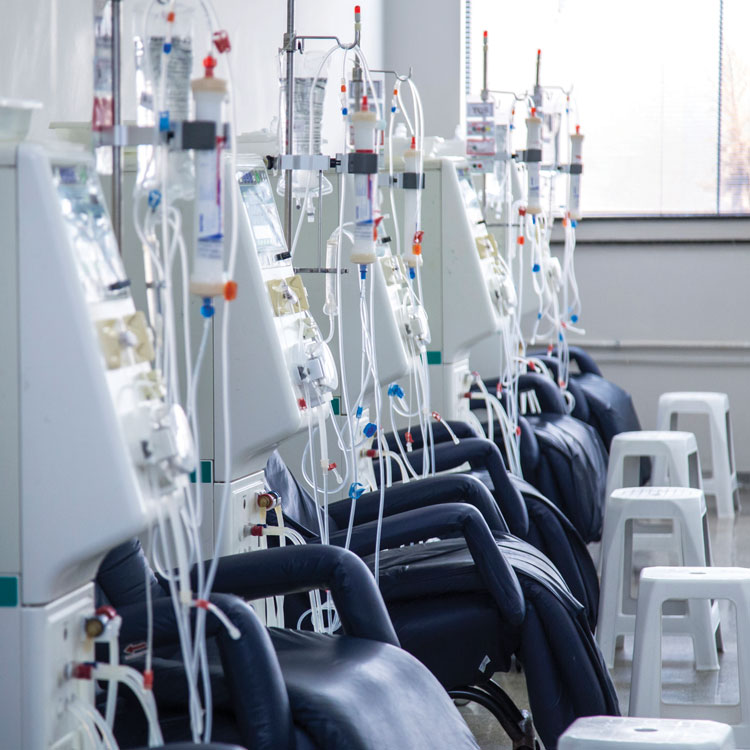
That includes a way to care for dialysis patients with hepatitis B completely separate from non–hep B dialysis patients—using a curtain for separation is not enough, warns Kathleen Good, MSN, RN, a former surveyor with TJC and now an associate of Patton Healthcare Consulting, which is based in Naperville, Illinois.
In a November 7 blog post, Andrew Bland, MD, MBA, MSAP, FAAP, FACP, medical director of TJC’s Division of Healthcare Quality Evaluation, wrote that among other infection control practices for hemodialysis, surveyors will be observing water and dialysate testing, medication storage, preparation and administration, and “patient placement in full view of staff during dialysis treatment.”
What this means, says Good, is that patients must be observable at all times for their safety. In particular, staff must be able to see “dialysis lines where they are connected to the bovine graft, AV fistula, intrajugular catheter, or Permacath™,” she says. Staff must also be able to hear and see the dialysis machines as patients are undergoing dialysis.
Patients with respiratory illnesses or fevers must also be kept at least six feet away, says Good. While a curtain in that case may be used as a barrier, the patient still shouldn’t be close to other patients. This guideline also applies to patients with skin wound drainage or fecal incontinence, to reduce the risk of transmission of infection, notes Good.
Isolate Hepatitis B patients
Patients diagnosed as positive for hepatitis B must be treated in a separate room, reiterates Good. “This is according to ESRD [end-stage renal disease] Conditions of Participation [CoP] for outpatient dialysis centers,” which Patton Healthcare Consulting recommends hospitals review when setting policies and procedures for dialysis.
“Hep B–positive patients should be placed in a separate room or separate area away from other non–hep B patients and taken care of by one nurse who does not take care of other hemodialysis patients,” says Good.
In a recent HCPro webinar on survey hot spots, including dialysis, Good recommended facilities should:
> Vaccinate all susceptible patients against hepatitis B
> Consider influenza (inactivated) and pneumococcal vaccinations for patients
> Conduct routine testing for hepatitis B and hepatitis C viruses
To prevent the spread of hepatitis B related to dialysis, Good recommended the following:
> Hospitals must dialyze hepatitis B (HBsAg+) patients in a separate room, using separate machines, equipment, instruments, and supplies. (HBsAg+ means a hepatitis B surface antigen in a lab test was positive.)
> Nurses or other staff treating patients must wear a separate gown with hep B patients.
Staff caring for hep B patients shouldn’t care for HBV-susceptible patients at the same time, including during the same shift or even during a patient changeover. (HBV-susceptible means anyone who has never been infected and lacks immunity to the hepatitis B virus, explains Good.)

Train staff on talking with surveyors
Ensure that nurses and other staff understand how to clean and disinfect the dialysis station, and that they know the procedures to prevent the spread of hepatitis B and other infections, says Good.
Among other things, according to the ESRD CoPs, you can expect CMS surveyors to ask the dialysis nurse:
> What the facility will do to prevent and control the spread of infections
> What the facility’s policies and procedures are regarding hepatitis testing and control among patients and staff
> How the staff collects and disposes of waste, including needles
> When and where protective clothing is worn, and where the clothing is stored during breaks
A.J. Plunkett is editor of the Simplify Compliance publication Inside Accreditation & Quality. She may be reached at aplunkett@blr.com.
