eConsults: Using Primary Care Providers as the Solution to Specialist Shortages
By Brooke LeVasseur
Our healthcare system uses primary care physicians (PCP) as the hub of care coordination. PCPs provide health promotion, disease prevention, health maintenance, counseling, patient education, diagnosis, and treatment of acute and chronic illnesses. Through routine checkups, primary care can identify and treat conditions early. As a result, adults in the U.S. who have a PCP are 19% less likely to die prematurely than those who only see specialists for their care (Starfield, Shi, & Macinko, 2005). Moreover, people who receive primary care spend 33% less on healthcare than people who only see specialists—in particular, by reducing the need for emergency room care, where costs are at least four times higher than other outpatient settings (Cox, 2015). Primary care, then, is becoming increasingly important to achieve cost and population health metrics within the shift to value-based care models.
The challenge ahead
PCPs are challenged to ensure that patients get the care they need in the right setting, from the most appropriate provider, and in a manner consistent with the patient’s desires and values. Complicating this already difficult task, an estimated 209,000 PCPs are caring for a population that is quickly approaching 325 million (AHRQ, 2018; U.S. Census Bureau, n.d.).
Not surprisingly, PCPs have gradually increased their referrals to specialist care; the number of specialist referrals has more than doubled in the United States since 1999 (Barnett, Song, & Landon, 2012). This increase has led to greater challenges for both PCPs and specialists. Common issues include referrals that lack complete medical workups, are sent to the wrong specialist, or are inappropriate for escalation to a specialist. Furthermore, there can be long delays before PCPs receive the results from specialist referrals, greatly decreasing the chances that a PCP can optimize a particular patient’s care or gain knowledge from the referral to treat similar cases in the future. The average wait time for results in five specialty areas, within top 15 major metropolitan areas, was over three weeks. Even seeing a specialist can be a major challenge—in some specialties, wait times for specialist appointments may reach up to a year (Merritt Hawkins, 2017). These referral issues can delay necessary care for patients, decrease their satisfaction with the care process, and drive up healthcare costs.
Lastly, a looming shortage of specialist physicians threatens to further hinder patient care. At a time when the U.S. is faced with a highly comorbid and aging population, the country is also projecting a deficit of 95,000 specialty physicians by 2025 (IHS, 2015).
Creating the ‘super PCP’ with telehealth resources
To overcome the issues plaguing care coordination between PCPs and specialists, PCPs must embrace tools and resources that extend their clinical domain without delegating patient care. This “Super PCP” capability is enabled by evolving telehealth solutions including eConsult platforms (also known as “eReferrals” and “virtual consults”) that create a peer-to-peer communication channel through which the PCP and specialist can confer, share the patient’s medical history, and collaborate on a care plan. With this approach, the patient remains in the capable hands of the PCP while benefiting from specialized medical expertise.
An eConsult is a simple process for PCPs and patients (Figure 1). During a typical office visit, the PCP documents the encounter within the EHR, logs the assessment and treatment plan, and cites the need for a specialist consult. The system extracts the necessary patient data to send to the relevant specialist, who provides the consult within a matter of hours. The PCP is then notified that the consult has been completed, and the patient returns to the PCP for follow-up or visits the specialist, as needed.
Figure 1: Basic Steps of an eConsult
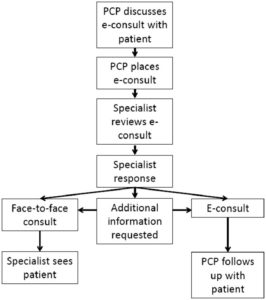
Dr. Christopher Dodd, chief care transformation officer at ConcertoHealth, observes: “When embraced, eConsults became a tool for providers to help them become a ‘Super PCP’ to serve as the sole provider to the patient.” Indeed, with technology seamlessly integrated into the organization’s workflow and electronic health record, a PCP can obtain the expert guidance of board-certified specialists on clinical questions, diagnostics, workup, and treatment recommendations, allowing the PCP to manage patient care that might not require a face-to-face visit with a specialist.
Dr. Dara Richards, chief medical officer of Southwest Community Health Center, championed the implementation of eConsults within her organization and noted both immediate and long-term advantages. “It was very eye-opening for our organization that we could receive such a rapid and thorough response from a specialist on a question or referral, usually within hours,” she says. In addition, Richards notes that each consult has lasting benefits. “With the education provided from specialist recommendations, providers were realizing that if presented with the same problem in the future, a referral would not be necessary.”
The benefits of ‘super PCP’ care
eConsults benefit patients, payers, physicians, and health systems. There is enhanced care coordination as a result of keeping the patient within primary care. eConsults allow for fewer appointments, less transfer of medical information, and shorter time from diagnosis to treatment. Patients benefit from consistent follow-up with the provider they know and trust; additionally, patients who could not otherwise access or afford to see a specialist can benefit from specialist consultation. For instances where a specialist visit is appropriate, appointments are available sooner because unnecessary appointments are not filling the specialist’s schedule.
eConsults benefit health insurers by keeping a higher percentage of patients within the primary care setting, thus significantly reducing costs. In addition to eliminating spend on unnecessary specialist visits, ensuring timely access to care can reduce wasteful ED visits and hospitalizations.
For physicians, eConsults are a clinically valuable resource to expand care capabilities and increase their own knowledge base. Fewer inappropriate referrals and more complete information sharing translate to higher patient satisfaction and retention. Physicians can also earn additional revenue by expanding their scope of care. Finally, health systems benefit from eConsults’ potential to improve access to specialty care within the primary care setting, strengthen population health initiatives and care coordination, and support quality metric initiatives.
Brooke LeVasseur is CEO of AristaMD.
References
AHRQ (2018, July). The number of practicing primary care physicians in the United States: Primary care workforce facts and stats no. 1. Retrieved from https://www.ahrq.gov/research/findings/factsheets/primary/pcwork1/index.html
Barnett, M. L., Song, Z., & Landon, B. E. (2012). Trends in physician referrals in the United States, 1999-2009. Arch Intern Med, 172(2), 163–170.
Cox, E. (2015, December 14). Why do we continue using the ER for care? US News. Retrieved from https://health.usnews.com/health-news/patient-advice/articles/2015-12-14/why-do-we-continue-using-the-er-for-care
IHS, Inc. (2015, March). The complexities of physician supply and demand: Projections from 2013 to 2025. Association of American Medical Colleges. Retrieved from https://www.aamc.org/download/426248/data/thecomplexitiesofphysiciansupplyanddemandprojectionsfrom2013to2.pdf
Merritt Hawkins (2017). Survey of physician appointment wait times and Medicare and Medicaid acceptance rates. Retrieved from https://www.merritthawkins.com/news-and-insights/thought-leadership/survey/survey-of-physician-appointment-wait-times
Starfield B., Shi, L., & Macinko, J. (2005). Contribution of primary care to health systems and health. Milbank Quarterly, 83(3), 457–502.
US Census Bureau (n.d.). U.S. and world population clock. Retrieved from https://www.census.gov/popclock
