Could Legally Mandated Racial Bias Training Reduce Maternal Mortality Rates for Black Women?
By Megan Headley
With maternal mortality rates for black women three to four times higher than their white counterparts—and the numbers for U.S. maternal mortality bleak across the board—legislators are stepping in to push for rapid improvements in maternal care.

A 2016 analysis of data published in Obstetrics & Gynecology showed a dramatic worsening in U.S. maternal mortality rates, increasing from 18.8 per 100,000 live births in 2000 to 23.8 in 2014. The researchers pointed out that this increase of nearly 27% took place in the United States while global rates fell by a third around that same time period. The data becomes even more pronounced when examining maternal mortality rates for black women. Data from the Centers for Disease Control and Prevention (CDC) on births between 2011 and 2014 revealed rates of 12.4 deaths per 100,000 live births for white women and 40.0 deaths per 100,000 live births for black women.
Public discussions around this disparity—from tennis star Serena Williams’ high–profile battle with complications after giving birth that care providers nearly ignored, to the death of Shalon Irving, a CDC epidemiologist and researcher on racial disparity, three weeks after the birth of her daughter—are now pushing legislators to demand change.
On August 22, 2018, Sen. Kamala Harris (D-Calif.) introduced the Maternal Care Access and Reducing Emergencies (CARE) Act (S. 3363) to reduce maternal mortality rates in general and, more specifically, eliminate racial disparities in maternal health outcomes. A corresponding bill was introduced in the House (H.R. 6698) on September 4 by Rep. Alma Adams (D-N.C.).
The text of the Maternal CARE Act states, “A growing body of evidence indicates that stress from racism and racial discrimination results in conditions—including hypertension and preeclampsia—that contribute to poor maternal health outcomes among Black women.” It cites as support the eye-opening CDC statistics, as well as a 2016 study by University of Virginia researchers that found “White medical students and residents often believed biological myths about racial differences in patients, including that Black patients have less-sensitive nerve endings and thicker skin than their White counterparts.”
Among the ways it seeks to drive change, Harris’ legislation proposes awarding $5 million grants from 2019 through 2023 to health professional training programs to support the development of evidence-based implicit bias training, with a priority on OB-GYN practitioners. In addition, the bill proposes funding up to 10 state-supported pregnancy medical home (PMH) programs, based on a model set by North Carolina.
North Carolina’s PMH program incentivizes maternal healthcare providers to provide integral healthcare services to pregnant women and new mothers. Launched in 2011, it now includes more than 350 state practices and 1,600 providers. Following the implementation of the program, the state saw its pregnancy-related mortality rate for black women drop from 5.1 times higher than that of white women in 2004 to a rate virtually identical to white women in 2013: just 24 deaths per 100,000 live births.
“The PMH program has been credited with the convergence in pregnancy-related mortality rates because the program partners each high-risk pregnant and postpartum woman that is covered under Medicaid with a pregnancy care manager,” the Maternal CARE Act states.
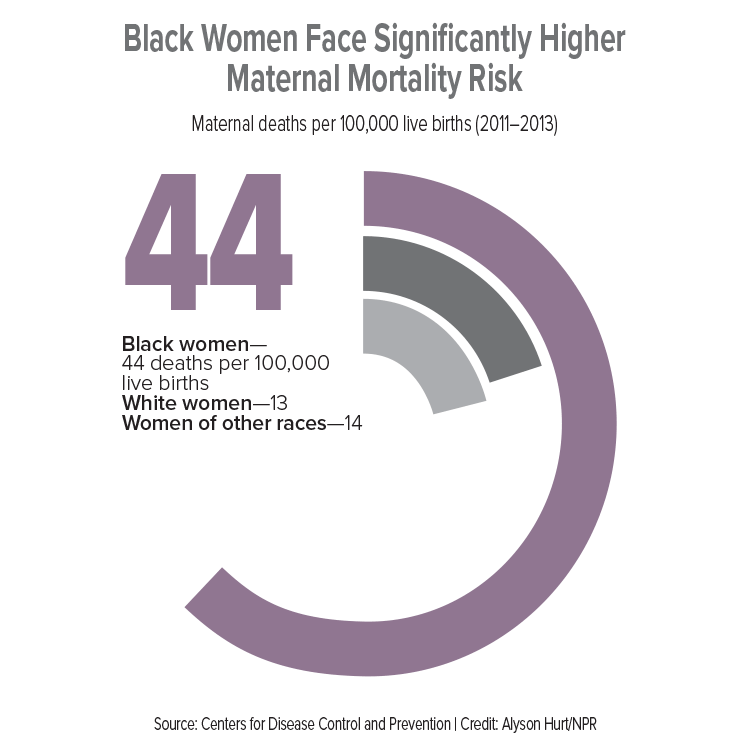
Harris’ bill also requests the National Academy of Medicine complete a study in bias recognition, with the goal of developing recommendations within three years for rolling out bias training to all medical schools and health programs.
But it’s the scarcity of federally tracked data on maternal mortality that has posed problems in making wide-scale improvements to maternal care. The Modernizing Obstetric Medicine Standards (MOMS) Act (S. 3392), proposed August 28, 2018 by Sen. Kirsten Gillibrand (D-N.Y.), aims to address this roadblock.
The legislation sets out to create the Alliance for Innovation on Maternal Health to spearhead a national data-driven maternal safety and quality improvement initiative, based on evidence-based best practices to improve maternal safety and outcomes. This department would assist states in developing postpartum safety and monitoring practices, based on the best practices the program developed, to be rolled out as a series of continually updated maternal safety bundles. It also would work to reduce state-by-state variations in maternity and postpartum care to eliminate preventable maternal mortality.
The MOMS Act proposes bundles addressing topics that would include the reduction of racial and ethnic disparities in maternity care, as well as improved care for women with substance abuse disorders; attention to maternal mental and emotional health; and overall strategies for empowering women before, during, and after childbirth to ensure better communication between patients and healthcare providers. Other topics might include safe reduction of primary cesarean birth; obstetric hemorrhage; maternal venous and thromboembolism; severe hypertension in pregnancy, including preeclampsia; postpartum care basics for maternal safety; severe maternal morbidity review; and support after a severe maternal morbidity event.
The MOMS Act would grant $25 million over five years to states and hospital systems in support of the legislation’s goals.
As of presstime, the Maternal CARE Act had been referred to the Senate Committee on Finance, while the MOMS Act sat with the House Committee on Health, Education, Labor, and Pensions.
Megan Headley is a freelance writer and owner of ClearStory Publications. She has covered healthcare safety and operations for several publications. She can be reached at megan@clearstorypublications.com.
