Being Creative, and the Importance of ‘Thinking Inside the Box’
By Robert F. Sharrow, AIA, ACHA, EDAC
Changing federal requirements, evolving business practices, the continuing coronavirus pandemic, and the uncertainty of federal regulations and payments are increasingly making access to capital—and therefore, building new facilities—difficult. Smaller, targeted projects are one result of these challenges, with design teams increasingly engaged in replacements of diagnostic and therapeutic equipment, renovations of operating rooms (OR), renovations or expansions to emergency departments, upgrades to IT systems, and renovations to support new clinical treatments and operations such as the construction of hybrid ORs.

Unique infrastructure challenges
Even these projects, however, can end up being more complicated and costly, especially when it comes to infrastructure upgrades. Electrical and HVAC updates are of particular importance to support new technology, which typically requires additional power and generates additional heat. Other important renovations include installing wireless systems and components used for collecting data or interacting with electronic medical records. This article offers insights into the challenges, solutions, and key considerations addressing infrastructure challenges posed by smaller, targeted healthcare projects.
Utilize a targeted strategy. Often, infrastructure changes and upgrades are needed, but it doesn’t make sense to upgrade the existing central electrical or mechanical equipment due to the high cost and possible service disruptions. However, even smaller projects such as adding a new piece of imaging equipment will require additional cooling. The most practical solution is to install a split cooling system connected to domestic cold water, chilled water, or an outdoor condenser capable of supporting a small department or series of rooms. Rather than upgrading a central piece of equipment, consider installing small package units to upgrade areas in an aging building. The limiting factor in this approach may be finding viable locations for the new equipment.
Make maintenance aware. Smaller, dedicated cooling units can pose a preventive maintenance challenge for facility staff. Also, package units added after a building is in use may not be indicated on original as-built drawings—only on the renovation drawings. As a result, if a long-term employee in facilities retires or leaves, an information gap could occur as new maintenance staff may not be aware of the more recently installed equipment until it fails. Regularly conducting systemwide performance reviews can help alleviate this situation.
Take a holistic approach. Before undertaking any renovation project, it is critically important that stakeholders and design teams study and assess the existing infrastructure to identify and understand exactly what is required to support the new space being considered. Is there enough supply air and exhaust? What about electrical power, plumbing waste, HVAC, fire alarms, IT, security, and other services? Can equipment be added close to the renovated area without having to upgrade the entire energy system? Developing a solution is best done through a team approach that includes experienced specialists—at minimum, a mechanical engineer, an electrical engineer, an architect, and a structural engineer—to analyze the impact of new heavy equipment.
Lessons learned from real-world solutions
Every project has unique elements, and there are no “one size fits all” solutions. The following examples illustrate how implementing the above planning suggestions can address infrastructure challenges posed by smaller, targeted healthcare projects.
Replacing older equipment with a new, more efficient system. Two orthopedic ORs at a large but older facility in Detroit had a high-velocity horizontal laminar flow system for orthopedic joint replacements. While the system was considered state-of-the-art when constructed in the mid-1980s, it took up an immense amount of space, required filters to be replaced, was noisy, and had reached the end of its usable life. For this project, the design team replaced the 40-year-old horizontal units and installed a new recirculating system, using the same amount of sterile air delivered from the central unit, so they did not have to go beyond the ORs themselves. A recirculating system with a fan and HEPA filters was mounted in the ceiling, resulting in a low-velocity, high-volume vertical laminar flow system delivering HEPA filtered air to the surgical field.
Opting for a less expensive custom design. An urban, tertiary care hospital needed to replace an aging air circulation system to support its large, high-volume OR platform helping transplant patients. Air sterility was a critical factor. The design team developed a custom air handling system with off-the-shelf components that increased air changes from 25 per hour to over 40 per hour at low velocity. While a custom design, this approach was less expensive than an entire system replacement.
Retrofitting to control pressure relationships. The same hospital needed to expand its catheterization labs into a former radiology file area that was no longer needed because its x-ray records had gone completely digital. While the square footage was adequate to accommodate the expansion, the air supply was not sufficient for the sterile environment required for a cath lab, and a new HVAC unit for highly filtered air was needed. The design team utilized the air supplied from the central HVAC system, and a smaller unit was also installed near the new cath labs to augment circulation for the two new rooms. With ventilation air coming from the existing central system, it was determined that air pressure was not adequately controlled, so a booster fan was retrofitted on the supply duct. This simple retrofit avoided the need to alter the entire existing HVAC system located in a central mechanical room, which would have been too disruptive to the rest of the hospital.
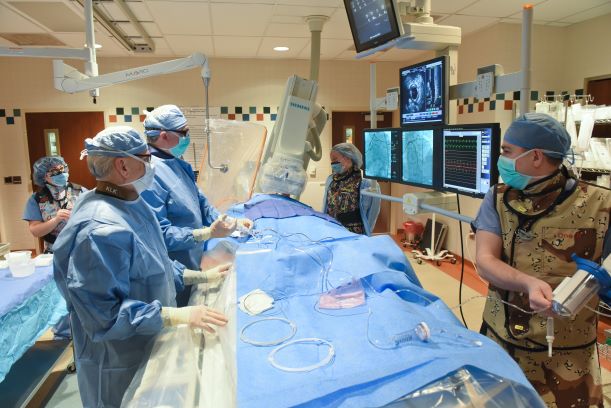
While smaller projects may be less expensive for hospitals, and thus currently more in reach than major replacement projects, they come with their own challenges and requirements that necessitate navigating the limitations imposed by existing infrastructure systems. Careful attention to the existing operations and infrastructure in a hospital will save both time and construction costs.
Robert F. Sharrow, AIA, ACHA, EDAC, is a senior vice president and director of healthcare planning at Albert Kahn Associates, Inc.
