Achieving Zero Preventable Deaths: One Hospital’s Journey
By Kimberly Chavalas Cripe and Joe Kiani
Every healthcare system and individual clinician wants the best possible outcomes for patients. A key component of clinical excellence is often the hospital’s level of commitment to a culture of safety and transparency. While Children’s Hospital of Orange County (CHOC) in California has long been a champion of patient safety at the regional, state, and national levels, it is always on the lookout for new opportunities to improve its patient safety outcomes.
At CHOC’s Quality Committee meeting in 2015, CHOC deliberately shifted its established goal from “reducing hospital-acquired conditions” to “achieving zero preventable deaths.” This goal became one of three quality domain factors that would determine annual leadership bonuses, thus further encouraging physicians to aggressively pursue it.
The quality and clinical leadership teams at CHOC designed a plan to achieve “zero” in concert with the Patient Safety Movement Foundation’s (PSMF) Actionable Patient Safety Solutions (APSS) (Agency for Healthcare Research and Quality, 2015). The APSSs are developed by teams of patient safety experts, healthcare technology professionals, and patient advocates, resulting in evidence-based processes that have been proven to reduce preventable deaths from medical errors (Makary & Daniel, 2016; Patient Safety Movement, n.d.). The PSMF provides 39 APSSs to overcome preventable deaths, including APSSs to address failure to rescue and healthcare-associated infections. PSMF offers the APSSs at no cost on its website, allowing hospitals to use them as a road map to eliminate preventable deaths.
In planning for zero preventable deaths utilizing the APSSs, CHOC conducted a rigorous hospitalwide audit to identify areas that could most benefit from improvement. To enhance its data reliability and accurately measure achievable outcomes, CHOC developed color-coded metrics to accompany each of the APSSs as a method to track progress (Figure 1).
Figure 1
Color-Coded Goals Progress Tracker
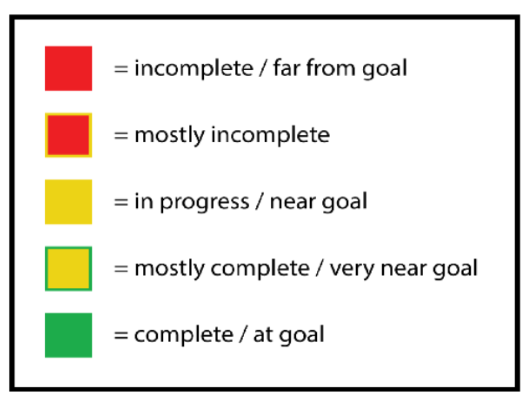
A series of mitigation documents was also developed to provide a systematic approach to address unexpected outcomes, including preventable patient harm or death. The mitigation process included root cause analysis to understand the sources of errors and provide full transparency and accountability among the healthcare team, patient, and family.
Following a thorough gap analysis, hospital staff were armed with a set of established targets and validated metrics that would measure progress across the organization. Fortunately, CHOC takes pride in continued safety process improvement, so it was relatively easy for the leadership team to communicate the advantages of implementing the APSSs. Although some units in the hospital were initially skeptical, they quickly recognized the positive outcomes resulting from the integration of the APSSs and embraced the new road map to improved patient safety.
Creating an environment of trust and transparency without fear of reprisal was another key factor to achieve success and improve patient safety (Leape et al., 2009). While all healthcare systems expect a safety mindset among their staff, the CHOC team advanced quickly on its safety journey because its new process made it safe to admit to mistakes and learn from them. The introduction of the Agency for Healthcare Research and Quality’s CANDOR (Communication and Optimal Resolution) program provided CHOC with a disciplined, transparent approach following adverse events (Lambert et al., 2016). The CANDOR “Seven Pillars” include:
- Create an open and transparent culture that encourages staff to speak up and self-report
- Report the event
- Investigate while supporting the involved caregiver
- Communicate with the patient and family
- Care for the patient and family through apology and resolution, including financial when appropriate
- Conduct event reviews and link them back to process improvements
- Collect data and complete tracking of information
As a result of CHOC’s enterprisewide commitment to achieve zero preventable deaths, the organization achieved transformational change. Over a period of 43 months, CHOC had zero preventable deaths and a dramatic reduction in preventable harm as of the date of this report. From 2013 to 2020, CHOC also had a significant decrease in the rate of serious safety events. In 2019, CHOC became the first pediatric facility to be named a five-star hospital by the PSMF for making commitments that aligned with all APSSs relevant to pediatrics. In the last three years, CHOC has significantly expanded its approach to include all APSSs applicable to pediatric care.
CHOC has achieved an impressive rise in its safety results through an openness to pursuing new safety policies and procedures, a successful implementation of PSMF’s APSSs, and a disciplined, transparent approach when adverse events occur. CHOC embraces this continuous process and remains committed to consistently searching for and implementing best practices among healthcare systems, hospitals, and clinicians in the pursuit of eliminating preventable patient death and harm (Chassin & Loeb, 2011).
Kimberly Chavalas Cripe is president and CEO of Children’s Hospital of Orange County (CHOC). Joe Kiani, BSEE, MSEE, is founder and chairman of the Patient Safety Movement Foundation and founder, chairman, and CEO of Masimo.
References
Agency for Healthcare Research and Quality. (2015, November). Efforts to improve patient safety result in 1.3 million fewer patient harms (Publication 15-0011-EF). U.S. Department of Health and Human Services. https://www.ahrq.gov/hai/pfp/interimhacrate2013.html
Chassin, M. R., & Loeb, J. M. (2011). The ongoing quality improvement journey: Next stop, high reliability. Health Affairs (Millwood), 30(4), 559–568. https://doi.org/10.1377/hlthaff.2011.0076
Lambert, B. L., Centomani, N. M., Smith, K. M., Helmchen, L. A., Bhaumik, D. K., Jalundhwala, Y. J., & McDonald, T. B. (2016). The “seven pillars” response to patient safety incidents: Effects on medical liability processes and outcomes. Health Services Research, 51(Suppl 3), 2491–2515. https://doi.org/10.1111/1475-6773.12548
Leape, L., Berwick, D., Clancy, C., Conway, J., Gluck, P., Guest, J., Lawrence, D., Morath, J., O’Leary, D., O’Neill, P., Pinakiewicz, D., & Isaac, T. (2009). Transforming healthcare: A safety imperative. BMJ Quality & Safety, 18(6), 424–428. https://doi.org/10.1136/qshc.2009.036954
Makary, M. A., & Daniel, M. (2016). Medical error—the third leading cause of death in the US. BMJ, 353, i2139. https://doi.org/10.1136/bmj.i2139
Patient Safety Movement. (n.d.). APSS blueprints. https://patientsafetymovement.org/actionable-solutions/actionable-patient-safety-solutions-apss/
