By Carl A. Patow, MD, MPH
In medical simulation, computer-controlled equipment advances medical learning and ensures that students learn procedures and treatment protocols before using them on actual patients. A simulation environment allows students and providers to learn, practice, and repeat procedures as often as necessary in order to correct mistakes, fine-tune their skills, and optimize clinical outcomes. In addition, with simulation, students and residents can gain experience with various types of patients and cases they may not actually encounter during their rotations and shifts. This is particularly significant for training in managing emergency situations. Patients with serious and volatile conditions may not get second chances.
Research studies indicate that simulation improves learning (Grantcharov, et al., 2004). Simulation is especially effective in developing skills in procedures that require eye-hand coordination and ambidextrous maneuvers, such as bronchoscopy. Simulation training helps learners prepare to deal with unanticipated medical events, develops teamwork and communication skills, increases confidence, and improves performance. Interest in the benefits of medical simulation is increasing, as evidenced by the establishment in January 2004 of a new multi-disciplinary, multi-specialty, international society, the Society for Medical Simulation (SMS), www.socmedsim.org. SMS represents the fast-growing group of medical educators and researchers who utilize a range of simulation techniques and technologies for education, testing, and research. The membership is united in its commitment to improve performance and reduce errors in patient care using all types of simulation including task trainers, human patient simulators, virtual reality, and standardized patients (volunteers who act out clinical situations).
HealthPartners is a family of nonprofit, consumer-governed healthcare organizations that include a 630,000-member health plan (covering nearly one in four residents of the Minneapolis-St. Paul metropolitan area), the 450-bed Regions Hospital, and the HealthPartners Medical Group, with 637 physicians at 28 primary care and specialty care clinics. Through its Institute for Medical Education (IME), HealthPartners is one of Minnesota's four largest providers of undergraduate, graduate, and continuing medical education. In conjunction with the University of Minnesota Medical School, HealthPartners trains more than 500 resident physicians in 16 medical specialties each year at Regions Hospital. IME also provides continuing medical education for HealthPartners physicians, nurses, and other medical professionals as well as providers from around the Midwest.
In May 2001, the Robert Wood Johnson Foundation and the Institute for Healthcare Improvement launched "Pursuing Perfection," a $20.9 million initiative to support efforts to transform healthcare in accordance with the principles set forth by the Institute of Medicine (IOM) in its landmark report, Crossing the Quality Chasm: A New Health System for the 21st Century (IOM, 2001). Seven finalists, including HealthPartners, each received two-year, $1.9 million grants to implement restructuring plans and to share their work with healthcare organizations across the country. Under HealthPartners' comprehensive Pursuing Perfection initiative, IME is responsible for increasing the effectiveness and safety of care delivery through graduate and continuing medical education programs.
In 2002, IME initiated discussions with the nursing department at Metropolitan State University about using available space at their campus for a medical simulation center for their nursing students, medical students in residency programs at Regions Hospital, and learners in HealthPartners' continuing medical education programs. Metropolitan State's St. Paul campus is a three-minute drive from Regions Hospital, where HealthPartners and the University of Minnesota train medical students and residents.
Together, HealthPartners and Metropolitan State designed and built a functioning medical simulation center in 12 months. The HealthPartners Simulation Center for Patient Safety at Metropolitan State University opened in April 2002. HealthPartners provided start-up funds to purchase $350,000 in simulation technology, with additional funding of $150,000 in 2003 and $100,000 in 2004, while Metropolitan State offered space and curriculum development services. Planned fundraising aims to add $800,000 to $1 million over the next three years to purchase additional simulation technology and for a permanent director, instructional design staff, and technology support staff.
Medical Simulation Technology
The equipment and simulation training procedures at the Simulation Center are designed to make learning realistic for students, residents, and providers. Five kinds of training are available at the Center:
Human Patient Simulators — The simulation technology centerpiece is a full-sized patient simulator that blinks, breathes, and has a heartbeat and pulse. Attached monitors display vital signs. It provides virtual simulation of almost every major bodily function. This simulator can be used for a range of scenarios from physical examination to major trauma. For instance, the virtual patient can be programmed to have a heart attack, with other sudden complications. The simulator even recognizes injected medications via a laser bar-code reader and responds with appropriate vital signs. It is particularly helpful for practicing the teamwork and communication required during heart attacks and other major clinical events. HealthPartners and Metropolitan State have added a pediatric human simulator and plan to introduce an obstetrics simulator in 2005.
Simulated Clinical Environments — An ICU/emergency room bay provides all the equipment for intubation, intravenous lines, and suction as well as a crash cart. Four examination rooms are available for practicing patient exams and communication skills. In addition, there are procedure skill rooms for venous catheterization and other procedures. A simulated operating room will open in 2005. It will support simulation training on sterile technique, surgical team roles and communication, and patient safety in the operating room.
Virtual Procedure Stations — A computer-controlled simulation device is available for teaching bronchoscopy, colonoscopy, and flexible sigmoidoscopy. Using these simulation programs, students insert the fiber-optic scope into a special computer console, designed to be anatomically realistic, instead of a real patient. Learners move the dials on the handpiece exactly as they would with a real scope, following their movements in real time on a detailed computer screen image of the lungs or colon. Students can examine and biopsy tissues, while "patient" responses are generated appropriately by the simulator's software. At the end of each session, the software assigns the learner a score based on technique and generates a report that helps track the student's progress over time and identify areas for improvement. Another simulator allows students to practice blood-drawing techniques, from skin cleaning and needle selection to puncture technique and aftercare.
| |

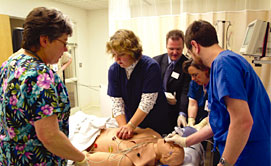 |
A nursing team from Regions Hospital in St. Paul practices emergency response on the human patient simulator.
Photo courtesy of HealthPartners Institute for Medical Education. |
Significantly, the simulators present a variety of different clinical scenarios that simulate many types of patients with different diagnoses and pathology. Therefore, students practice much more than procedure technique; they learn to apply their skills in a range of realistic clinical situations.
Electronic Medical Record (EMR) — As more healthcare organizations adopt EMRs to track patients and alert providers to their needs, providers require training to learn to use the systems. A fully functional EMR is provided in the four clinical exam rooms, complete with fictional patient histories, notes, and lab results.
Performance Recording — As of June 2004, the Center added video cameras and microphones in each of the major teaching areas, with a connection to a wide-screen monitor in a conference room. Observers in the conference room can watch a learning activity and offer feedback. Learners also have the opportunity to watch recordings of their learning activities to observe their performance and identify opportunities for improvement.
Simulation Learning for Emergency Medicine Residents
The traditional process of clinical education in emergency medicine, like other specialties, relies on learning and practicing diagnostic, therapeutic, and procedural skills on real patients. Computer-controlled simulation is now opening up new educational applications that show considerable promise in emergency medicine (Small et al., 1999; Reznek, Harter, & Krummel, 2003). This is evident at the HealthPartners Simulation Center.
The emergency medicine (EM) residency program at Regions Hospital was established in 1994, and the first class of residents began their training in 1996. The Regions EM residency has graduated 38 residents from 17 different medical schools, and they now practice in 14 states. Nine physicians begin their three-year EM residency annually at Regions.
According to Felix K. Ankel, MD, assistant professor of emergency medicine and residency director, excellence in patient care requires a combination of knowledge, skills, and attitudes. Medical educators tend to focus on knowledge, because it is the most straightforward component to teach and test. Thus, acquisition of skills and cultivating essential attitudes traditionally come in on-the-job training. Experiential learning is essential, and simulation enhances this aspect of the EM residency program (Ankel, 2004).
Residents spend 30 to 40 hours per year at the Simulation Center. That equates to five emergency room shifts annually. Cullen B. Hegarty, MD, is the assistant EM residency director at Regions and also serves as the director of medical student education and director of medical simulation. He uses the technology of the Simulation Center to teach basic procedural and patient management skills (Hegarty, 2004). The adult and pediatric human simulators are used to conduct a variety of different trauma and resuscitation scenarios, which include procedures such as establishing emergency airways. Residents also practice setting up central lines in the venous catheterization procedure room and utilize the bronchoscopy simulator.
Exposing residents to common emergency medicine cases, such as strokes, early in their training enables them to ascend the learning curve faster. In addition, Hegarty believes that simulation plays a critical role in supplementing experiential learning that residents derive during their emergency room shifts. Residents can be introduced to low-frequency, high-risk adult cases, such as rare toxicities, that they might not see and experience in the real emergency room. And most critical care patients are adults. Thus, the pediatric simulator offers indispensable experience in managing cardiac arrests in children and pediatric trauma. Hegarty and his colleagues are designing new applications of simulation. These include teaching advanced pediatric airway procedural skills with the bronchoscopy simulator and immersing residents in a range of toxicology cases and scenarios using both human simulators.
Emergency medicine residents have to learn to make quick decisions with limited data while responding to unexpected events. At Regions, a substantial portion of that experience is gained, without risk to patients, in simulation training. They must also learn critical care team management. Hegarty and Ankel immerse junior and senior residents in increasing complex clinical scenarios so that they have the opportunity to learn teamwork and develop their ER team leadership skills in realistically complex, challenging, and stressful emergency situations. It is in the evaluation of team leadership and performance that the Center's audiovisual technology is especially useful. Whereas it is difficult, and often impractical, to review cases in the emergency room during their busy shifts, at the Center residents go to a classroom to replay tapes of simulated scenarios. Faculty and the residents review, discuss, and critique the case management process. In Hegarty's experience, these sessions are effective in helping residents see that orders in the emergency room must be directed and clearly communicated to a specific team member who implements them and provides prompt feedback when the task is completed. Simulation training is thereby used not just to teach and practice procedural skills but to teach the residents to function in teams and to lead them.
A major focus of the Pursuing Perfection quality improvement initiative at HealthPartners is to put evidence-based best practices into practice. As guidelines and care pathways become increasingly important in the practice of emergency medicine, simulation is proving to be useful and effective in teaching and practicing protocols. Residents see and learn the workflow steps of various protocols (including managing chest pain, strokes, pneumonia, and sepsis), experience the logic of protocols, and internalize the policies. Simulation training reinforces fastidious attention to deal.
How do the emergency medicine residents respond to simulation learning? According to Ankel and Hegarty, it is clear that the residents experience the tension and feel the pressure of dealing with seriously ill patients in crisis situations in the simulation scenarios. They appreciate the chance to simulate cases that they may not see in their emergency room shifts,
as opposed to just reading about them in textbooks and hearing about them in lectures. Most of all, they value opportunities to make mistakes and learn from them in a safe educational environment.
Simulation Learning for CME and CE
Simulation learning is proving to be useful in continuing medical education. Carson Harris, MD, director of emergency medicine toxicology education at Regions, teaches Fundamentals of Critical Care at the Center. He adapted this standard curriculum for simulation and has become an enthusiastic supporter of simulation. He teaches his class to groups of ICU and CCU nurses who are training to work in emergency rooms. Harris believes the human simulator is a much more effective tool than a mannequin when it comes to learning procedures such as intubation.
| |

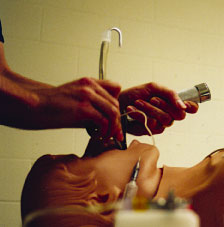 |
Simulation is used to teach skills like airway management and to integrate those skills into complex and realistic patient scenarios.
Photograph by Renee Whisnant, courtesy of Minnesota Medicine. |
Many practicing physicians may recall practicing intubation with a mannequin, an "Airway Annie." The difference with computer-controlled simulation is the realism. Learners feel the pulse and hear the breath sounds. The simulator responds to medications, and teams have to react to unfolding clinical scenarios and unexpected events in real time. Harris and Ankel explain the difference metaphorically — using a mannequin is like playing a video game in which one plays at flying an airplane; the human simulator is like getting into a full-fledged flight simulator.
Healthcare organizations across the nation are coping with the severe nursing shortage. Some 70 percent of all hospital chief executives reported in October 2004 that their facilities were experiencing shortages (AACN, 2004). When they do hire new nurses, how many healthcare organizations have tested their competency before they start treating patients? HealthPartners uses the Center for new employee orientation for all new HealthPartners Medical Group nurses. Clinic nurses use the catheter simulation equipment to practice and demonstrate intravenous access skills. Nurses new to critical care and step-down units are introduced to advanced clinical situations using the human patient simulator. Evaluating the skills of newly hired nurses, and helping them improve their skills when necessary, promotes patient safety.
Challenges
A key to the success of simulation training is integrating it into traditional education programs. Training in a simulated environment is a new, additional step in the learning process — a step between classroom instruction and actual clinical instruction with real patients. For some faculty it can be difficult to translate lecture material to a hands-on simulation environment. When faculty try the simulators themselves, they can more readily envision how to incorporate virtual training.
It is essential to engage clinical faculty early in the process of developing a simulation training program. Champions and early adopters who see the potential in virtual reality learning and who are willing to invest time and energy to create curriculum for the new learning environment are a great asset. Engaging the broader medical community in developing simulation centers is another key to success.
Another challenge is the speed at which technology and medicine are changing today. The human patient simulator and other technology in the Center may be obsolete within five years. Some of the equipment will be upgraded under warranty by manufacturers, but some will not. Thus, continuous funding and stable sources of financial support are necessary to keep pace.
Simulation is an important solution to the challenges of patient safety. Clearly, every individual healthcare organization need not, and cannot, develop its own simulation center. For advanced clinical simulation, the capital requirements at start-up are substantial. On a regional basis, building partnerships among health plans, hospitals, and medical education organizations to establish simulation centers is an appealing and practical option to consider. The benefits? Enhanced and more effective professional education and greater patient safety.
Carl Patow (carl.a.patow@healthpartners.com) is executive director, Institute for Medical Education at HealthPartners, and co-director of the HealthPartners Simulation Center for Patient Safety at Metropolitan State University. He graduated from the University of Rochester School of Medicine and received a master of public health degree from Johns Hopkins University.
References
Grantcharov, T.P., Kristiansen, V.B., Bendix, J., Bardram, L., Rosenberg, J., & Funch-Jensen, P. (2004) Randomized clinical trial of virtual reality simulation for laparoscopic skills training. British Journal of Surgery, 91(2), 146-150.
Institute of Medicine, Committee on Quality of Health Care in America. (2001). Crossing the quality chasm: A new health system for the 21st century. Washington, DC: National Academy Press.
Small, S.D., et. al. (1999). Demonstration of high-fidelity simulation team training for emergency medicine. Academic Emergency Medicine, 6(4), 312-323.
Reznek, M., Harter, P. & Krummel, T. (2002). Virtual reality and simulation: Training the future emergency room physician. Academic Emergency Medicine, 9(1), 78-87.
Interview with Felix K. Ankel, MD, conducted by David Aquilina (September 14, 2004).
Interview with Cullen B. Hegarty, MD, conducted by David Aquilina (September 27, 2004).
American Association of Colleges of Nursing (AACN) (2004). Retrieved on November 23, 2004, from http://www.aacn.nche.edu/Media/shortageresource.htm#about.




