 |
 |
 |

July / September 2004

Information Systems
Web-Based Tools
Aid Quality Improvement Projects

By Sanjaya Kumar, MD, MSc, MPH
Clinicians naturally seek improvement and evaluate alternate ways to provide appropriate and optimal care for their patients. While many healthcare organizations have embraced TQM (total quality management), Six Sigma, PDCA (Plan, Do, Check, Act), and other data-driven methodologies for conducting, achieving, and sustaining quality improvement (QI) and performance improvement (PI) projects, the rigor of data collection, aggregation, and statistical analysis�coupled with organizational resource constraints�has limited the scope and impact of those projects.
The application of Web-based information technology (IT) and data analysis tools to the QI process enhances the capability and capacity of leading healthcare organizations to conduct QI/PI projects and gain actionable knowledge for informed decision-making from them faster and without additional resource expenditure.
Case studies that accompany this article highlight how organizations have leveraged such IT solutions to extend and enhance their quality improvement programs in the areas of patient safety, staffing effectiveness, and clinical outcomes. In addition, these examples demonstrate how automating quality improvement processes can bolster decision-making throughout the organization.
The Burden of Performance Improvement
By definition, data-driven approaches to improving quality and performance require collection, aggregation, and analysis of data. The required data is specific to the objectives of the project. The data is computed according to a defined set of measures that allow periodic and continuous monitoring of the impact of implemented interventions. As healthcare PI professionals know, collecting data to meet various requirements mandated by the Joint Commission on Accreditation of Healthcare Organizations (JCAHO) as well as state and federal agencies alone represent a considerable burden on even the most robustly staffed quality departments.
Healthcare organizations that must collect, aggregate, and analyze data manually may be forced to limit the number and scope of quality improvement projects in which they can participate. Further, healthcare organizations are often missing "pieces" of their projects by necessity and not choice.
Projects that involve aggregating and analyzing data may require staff specially trained in mathematics and statistics. Staff shortages and budgetary constraints mean that only a limited number of staff members are certified or have extensive experience in designing and running performance improvement projects. Although some organizations use administrative helpers, volunteers, interns, and students to do data collection "grunt work," qualified performance improvement professionals are required to properly design, manage, and analyze the results from each project. These skilled professionals often represent the constraining factor that limits the number and depth of projects that an organization can conduct at any given time.
Once data has been collected, aggregated, and analyzed, the results must be transformed into a presentable format and disseminated, which requires considerable manual resources. Web-based technology platforms allow for seamless, integrated delivery of desired reports and project-related information to users with requisite access rights and privileges.
Easing the Burden
Incorporating Web-based information technology into quality improvement can greatly reduce the burden of conducting quality and performance improvement projects, disseminating findings, and implementing and tracking their progress. Information technology tools can extend and enhance the ability of a quality/performance improvement department to take on more projects, make a project more comprehensive, and involve appropriate stakeholders and decision-makers to effect change from across the organization.
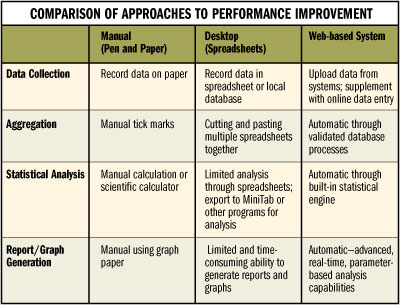
While almost all healthcare organizations have largely replaced "pen and ink" with desktop spreadsheets, databases, and statistical analysis tools such as Microsoft Excel, Access, and MiniTab, Web-based and Web-enabled tools provide greater capacity to achieve efficiency in collecting and analyzing data and disseminating results. While experienced statisticians might be able to calculate parameters like mean, median, mode, standard deviation, and variance in a matter of minutes, IT systems place the capability for on-demand statistical analysis in the hands of less experienced staff. In fact, by establishing automated data feeds from existing systems such as billing, payroll, and electronic medical records (EMRs), quality professionals can limit or sometimes eliminate the need for manual data collection.
Achieving Results
In addition to reducing the burden of quality improvement, information technology can help healthcare organizations achieve their performance improvement goals more successfully�and in less time. Poor or questionable data quality, long lag times between data collection and availability for presentation, and lack of buy-in from all stakeholders represent key factors that hinder quality improvement professionals from achieving results.
Sharing the Responsibility
When investing in these applications, healthcare organizations should avoid shifting the burden of performance improvement projects to the burden of implementing and maintaining cumbersome IT systems. While in the past IT leaders were the primary decision-makers for all IT purchases, end users now have a much greater hand in selecting applications. With their greater role in application selection, however, comes greater responsibility for understanding the impact of those decisions. There are some common questions that quality improvement staff should ask when evaluating the burden of support for IT applications:
- Is this application Web-enabled (resides on client server) or Web-based (requires nothing more than a browser for access)?
- What are the software, hardware, and IT staff requirements for this application?
- Does the system interface with other in-house legacy systems? What will be involved in building and maintaining these interfaces?
- How will system upgrades be handled? What effort will be required? Will data be lost or access to the application be interrupted?
Expanding the Role of the Quality Department
The next frontier in the application of information technology to quality improvement is in the seamless linkage of enterprise-wide quality improvement efforts to real-time executive dashboards. While many PI departments periodically share progress in quality improvement projects and focus reviews with leadership at monthly or quarterly meetings, some progressive healthcare organizations are providing their leadership with continuous feedback on critical organizational metrics. The process of transforming the role of the quality department from one of a report generator to one that supports informed decision-making for leaders at all levels requires both cultural change and the information technology to support the seamless (and secure) distribution of real-time information structured in a way that is useful.
Conclusion
Information technology helps healthcare organizations perform quality improvement activities both more successfully and more efficiently. Automating manual data collection, analysis, and presentation activities frees quality improvement professionals to investigate more, investigate deeper, and commit limited resources to achieving results�in less time. Information technology supports the goal of establishing a culture that prioritizes continuous quality improvement at all levels. In the words of Doreen Maples, the director of quality, risk, and HIM at ValleyCare, a multi-facility health system in the San Francisco Bay Area, "Our goal is to establish an environment where department managers have the tools to identify and fix systemic problems�versus relying on a 'quality department' to identify and report to them what issues have been identified."
Case Studies
- Missouri Hospital Association: Reducing the Burden of Public Reporting

- Easing the Burden of Accreditation and Compliance Requirements

- Using Information Technology to Improve Data Quality and Speed Feedback

- From Reports to Continuous Feedback: Real-Time Dashboards
Sanjaya Kumar, MD, MSc, MPH, is chief medical officer and chairman at Quantros, Inc., in Milpitas, California. Quantros provides and serves a broad range of quality oversight and data management needs for hospitals, managed care organizations, and pharmaceutical and biotechnology companies. Previously, Dr. Kumar was the designated clinical projects specialist for the Louisiana QIO (under contract from the Centers for Medicare & Medicaid Services), working to design and implement national- and state-based quality improvement (CQI) projects. Dr. Kumar is an internist by training, an epidemiologist, and holds a master's degree in health planning and financing. Dr. Kumar may be contacted at skumar@quantros.com.

|
 |
 |
 |


















|
 |



